Introduction
The impossibility to predict fluid responsiveness in hypotensive patients leads to negative outcomes and affects the quality of care. To address this problem, it is important to implement such intervention as passive leg raising (PLR) that can be used to maintain cardiac function (Rex et al., 2004; Teboul, Monnet, & Richard, 2005). The purpose of this paper is to discuss how this intervention can be implemented based on a specific change model, provide a rationale for using it, describe stages to complete, and evaluate its effectiveness.
The Selected Model and Rationale
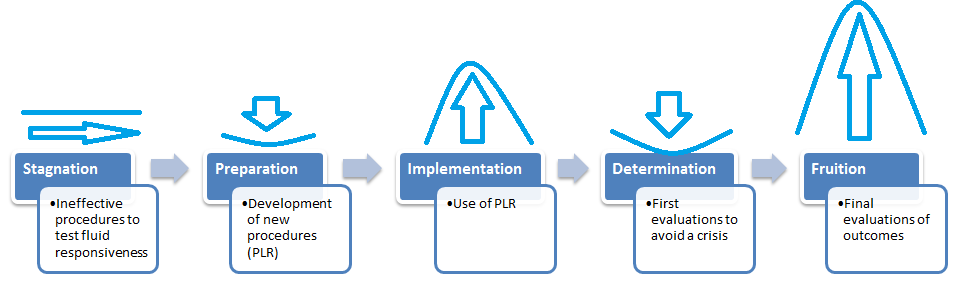
A change model selected for this project is Jeanie Daniel Duck’s Change Curve (Melnyk & Fineout-Overholt, 2014). The proposed intervention is based on changing the procedure of testing patients’ fluid responsiveness to avoid fluid overload (Cherpanath et al., 2016; Monnet et al., 2016). The hospital administration is oriented to implementing this change, and nurses should receive specific training. To integrate this intervention into clinical practice, it is appropriate to use Duck’s Change Curve model because, defining such stages of the change implementation as stagnation, preparation, implementation, determination, and fruition, the author refers to not only strategies but also to stakeholders’ reactions and perceptions of the change (Appendix A). The author represents these changes as a curve, and this approach is important to demonstrate what stages will be completed by nurses when they use PLR in the selected facility.
Application of the Model to the Implementation Plan
During the stagnation stage, nurses in the selected facility use traditional methods for working with hypotensive patients. They perceive this approach as appropriate, but it is ineffective and threatening to patients because of the risks of fluid overload (Monnet & Teboul, 2015; Pinsky, 2015). During the preparation stage, the principles of using PLR in the facility should be determined, and guidelines should be clearly formulated for nurses to use at the next stage. Nurses can demonstrate anxiety because of the necessity to participate in training sessions. The next stage is implementation, and stakeholders can demonstrate different levels of readiness to participate in the project. Thus, nurses should be educated regarding the importance of the intervention to improve outcomes for hypotensive patients (Monnet, Marik, & Teboul, 2016).
At the determination stage, stakeholders assess the first results. The risks of a crisis in promoting the change are high. For this intervention, it is important to complete the first evaluation after the second month to demonstrate how the change contributes to the process. At the fruition stage, the hospital administration will evaluate outcomes. Positive changes in predicting fluid responsiveness and stabilizing blood pressure in hypotensive patients are expected.
Conclusion
Duck’s Change Curve model is effective to support the proposed intervention in the selected facility. This model explains feelings and emotions typical of stakeholders at each stage of the process and strategies to use in order to address certain barriers. Applying the intervention to clinical practice with the help of this model, it is possible to expect that nurses will successfully use PLR for working with hypotensive patients.
References
Cherpanath, T. G., Hirsch, A., Geerts, B. F., Lagrand, W. K., Leeflang, M. M., Schultz, M. J., & Groeneveld, A. J. (2016). Predicting fluid responsiveness by passive leg raising: A systematic review and meta-analysis of 23 clinical trials. Critical Care Medicine, 44(5), 981-991.
Melnyk, B. M., & Fineout-Overholt, E. (2014). Evidence-based practice in nursing and healthcare: A guide to best practice (3rd ed.). Philadelphia, PA: Lippincott Williams & Wilkins.
Monnet, X., Cipriani, F., Camous, L., Sentenac, P., Dres, M., Krastinova, E.,… Teboul, J. L. (2016). The passive leg raising test to guide fluid removal in critically ill patients. Annals of Intensive Care, 6(1), 46-58.
Monnet, X., Marik, P., & Teboul, J. L. (2016). Passive leg raising for predicting fluid responsiveness: A systematic review and meta-analysis. Intensive Care Medicine, 42(12), 1935-1947.
Monnet, X., & Teboul, J. L. (2015). Passive leg raising: Five rules, not a drop of fluid! Critical Care, 19(1), 18-22.
Pinsky, M. R. (2015). Functional hemodynamic monitoring. Critical Care Clinics, 31(1), 89-111.
Rex, S., Brose, S., Metzelder, S., Hüneke, R., Schälte, G., Autschbach, R.,… Buhre, W. (2004). Prediction of fluid responsiveness in patients during cardiac surgery. British Journal of Anaesthesia, 93(6), 782-788.
Teboul, J. L., Monnet, X., & Richard, C. (2005). Arterial pulse pressure variation during positive pressure ventilation and passive leg raising. Functional Hemodynamic Monitoring, 3(2), 331-343.
Appendix A
Conceptual Model