Introduction
The main objective of this segment is to apply the Diffusion of Innovation Theory to the evidence-based practice (EBP) intervention of minimizing the prevalence of ventilator-associated pneumonia in intensive care settings. Justifications for using the model are also provided, along with the needed interpretations.
Diffusion of Innovation Theory
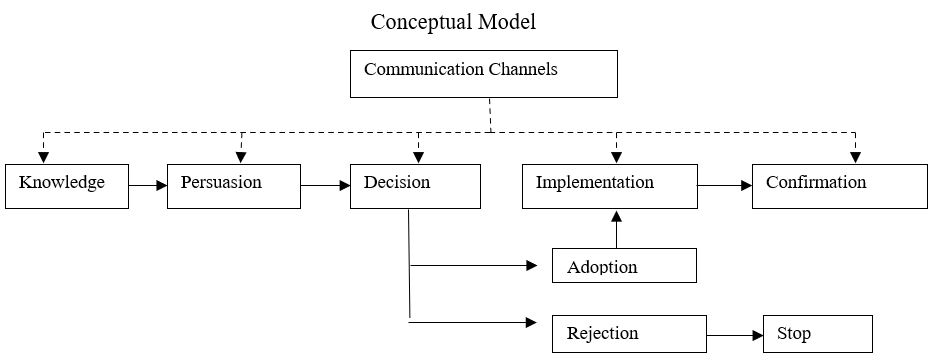
Available literature demonstrates that “the Diffusion of Innovation Theory supports the incorporation of capacity, infrastructure, facilitation, context, and evidence, and provides a framework for planned organizational change necessary to implement and sustain EBP” (Schultz, 2007, p. 12). The model is applicable in the present contexts as it ensures an enabling environment for the project facilitator and other stakeholders to diffuse the knowledge on the bundled practices across the social system (ICU) with the view to enabling nurses to implement practices that would substantially minimize the prevalence of ventilator-associated pneumonia in clinical settings (Andrews, Tonkin, Lancastle, & Kirk, 2014). The main stages of the model and their justifications are provided as follows:
The Knowledge Stage
In this initial stage, the individual and the healthcare organization must be exposed to the proposed intervention of using bundled practices to minimize the prevalence of ventilator-associated pneumonia in intensive care settings. Here, “the change agent (facilitator) must be prepared to answer questions regarding the what, why, and how of the proposed change” (Schultz, 2007, p. 12). The justification of this phase is anchored on the fact that it will provide the facilitator with the opportunity to use typical steps in the EBP process (e.g., developing PICOT questions, gathering baseline data, assessing research studies to note the strength of evidence, and preparing synthesis tables) to collect knowledge and evidence that will be shared across the unit with the view to gaining the support of other relevant stakeholders during the subsequent stage.
The Persuasion Stage
In this stage, individuals and other stakeholders in the unit/organization will develop an opinion about the proposed intervention by asking questions that can determine the feasibility and application of the intervention. This stage is useful as it allows the facilitator to discuss the benefits of the intervention to the unit, how it will achieve compatibility with the practice environment, and how outcomes will be observed. The stage will also help the facilitator to translate the evidence gained on the bundled practices into a practical guide that will oversee the implementation of the change effort (Dingfelder & Mandell, 2011).
The Decision Stage
In this stage, the EBP intervention will be pilot-tested in the ICU with the view to monitoring how the intervention is working and evaluating if the outcome change is a result of the piloted solution or other external variables. This stage will allow the facilitator and other stakeholders to make an informed decision on whether the practice change should be implemented fully or rejected based on the noted outcome change. Additionally, the stage allows the facilitator to train/educate other staff members on the practice change and also to collect and analyze data on how the bundled practices can minimize the prevalence of ventilator-associated pneumonia in the ICU (Keele, 2012).
The implementation Stage
Once the bundled practices have been adopted, the facilitator will use new team members and nurses to diffuse the practice change across the unit/organization with the view to enhancing uptake. Here, the facilitator and other members must consider the unit’s/organization’s structure, infrastructure, culture, or environment to ensure optimal diffusion of the practice change (Melnyk & Fine-Overholt, 2015). The justification of this phase is nested in the fact that it provides the facilitator with the opportunity to roll out the bundled practices across the unit and also to continuously monitor the intervention and associated outcome of reducing the prevalence of ventilator-associated pneumonia.
The Confirmation Stage
This stage of the model encompasses the incorporation of the practice intervention “as an approved written procedure with sign-off by all the disciplines involved in the change” (Schultz, 2007, p. 14). The stage will provide the facilitator with the opportunity to incorporate the outcomes of the bundled practices into the standard operating procedures of the ICU with the view to facilitating acceptance of the change and ensuring that data are constantly collected and assessed.
Conclusion
This section has not only discussed the implementation of the bundled practices EBP solution through each of the stages of the Diffusion of Innovation Theory, but also provided justifications for use and interpreted the theory in relation to the implementation plan for the EBP intervention.
References
Andrews, V., Tonkin, E., Lancastle, D., & Kirk, M. (2014). Using the diffusion of innovations theory to understand the uptake of genetics in nursing practice: Identifying the characteristics of genetic nurse adopters. Journal of Advanced Nursing, 70, 878-893. Web.
Dingfelder, H.E., & Mandell, D.S. (2011). Bridging the research-to-practice gap in autism intervention: An application of diffusion of innovation theory. Journal of Autism & Developmental Disorders, 41, 597-609. Web.
Keele, R. (2012). Nursing research and evidence-based practice: Ten tips to success. Burlington, MA: Jones and Bartlett Publishers.
Melnyk, B.M., & Fine-Overholt, E. (2015). Evidence-based practice in nursing & healthcare: A guide to best practice (3rd ed.). Baltimore, MD: Lippincott & Wilkins.
Schultz, A.A. (2007).Implementation: A team effort. Nursing Management, 38, 12-14. Web.