Introduction
X-ray is an image created on a specialized photographic picture that enables a doctor to identify various illnesses and injuries. This image is produced with the help of the x-ray machine, and these rays penetrate the body to reflect diseases of inner organs and bones. There are multiple benefits of using x-ray in medical imaging, for example, painless methods of diagnosis. Moreover, this procedure is relatively fast and enables a doctor to make a precise diagnosis. However, it is also important to note that some adverse outcomes are possible among these advantages. It is suggested that x-rays can be dangerous for people because of radiation. Indeed, it is crucial to examine how the x-ray machine works, the advantages and disadvantages of the x-ray method, and special considerations for patients.
The aim of a radiology practice is the generation of a report based on a medical radiograph. The clinical radiograph is a mechanism that enables the doctor to conduct radiological examinations, for instance, chest x-ray investigation (Syeda-Mahmood et al., 2020). It is essential to develop the area of radiology studies to improve the quality of delivering medical services and reduce possible outcomes from x-ray usage. Therefore, this paper will use various scientific pieces of research to demonstrate the work of x-ray devices and their influence on the organism of a human.
Mechanism
According to several sources, the x-ray was invented accidentally because of an experiment by physicist Wilhelm Roentgen. He discovered the technology while experimenting with gas tubes and electrons (Concerning Reality, 2019). He first noted that the paper receives a darker shadow under the influence of x-rays; he got an image of his hand bones in the form. This discovery became a significant innovation, as nobody managed to get a picture of bones and inner organs in an alive person before it. Through the years, the technology was improved and let many doctors see injuries and diseases in tissues and organs.
The x-ray machine is helpful in the examination of the head, neck, and extremities. It is possible to think of x-rays as light rays, which are relatively safe for the environment and human beings (Concerning Reality, 2019). X-rays are produced by moving electrons within atoms; these rays pass through the body. The solid matter can adsorb some x-ray radiation dose, but it mostly passes through the body and disappears. The passing-through radiation reaches the x-ray detector, and the pattern of this radiation that hits the machine is adapted to generate an image.
The patient is placed so that the required body fragment is positioned in front of the x-ray machine. When the doctor turns on the x-ray machine, the rays go through the body, and various body parts adsorb them in different amounts. Moreover, the medical x-ray image depends on the density of tissues and the number of protons in the nucleus of an atom or atomic number (NIH, 2021). An atomic number is a number in the periodic table which shows the number of electrons in the atom. For instance, dense structures as bones contain calcium which has a higher atomic number than most other tissues. Due to this trait, bones can adsorb x-rays quickly and create high contrast in the medical x-ray image. In contrast, soft tissues like fat, lungs, and muscles are less dense and create gray photos. Therefore, they are less visible to the x-ray machine, but still, all tissues are seen and penetrated by x-rays.
X-ray Lasers
Overall, x-ray lasers are machines that can produce x-ray radiation. X-ray lasers are used to examine cells, membranes, and cell structures. The most prominent device that can generate images is the European x-ray electron laser (Sanchez-Gonzalez et al., 2017). This machine is subject to multiple scientific studies and is one of the most successfully studied among other free-electron lasers. These specialized machines produce ultra-short impulses of x-ray radiation of high brightness. For instance, the range of x-ray laser machines can be modified depending on the target of the studied object. It is possible to adjust the intensity of impulses of an x-ray laser to diagnose a particular thing (Sanchez-Gonzalez et al., 2017). Therefore, per the required result, specialists may regulate the intensity of laser radiation produced.
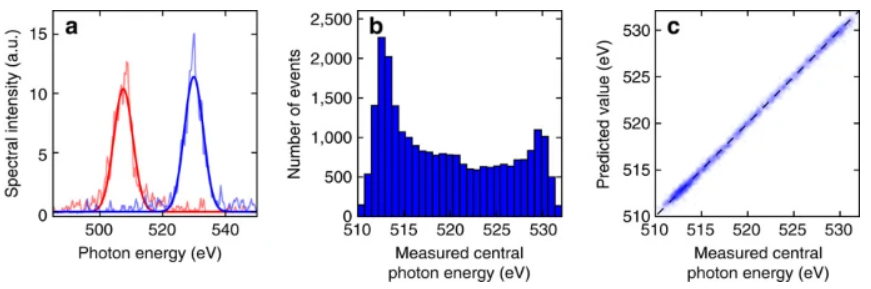
Moreover, x-ray lasers are high-speed and allow machines to produce images in a short spectrum of time. For instance, the x-ray laser machine can generate a shot in the range of one picosecond to several femtoseconds (Sanchez-Gonzalez et al., 2017). These time slices are the tiniest fraction of a second, and it allows to get an image instantly. However, x-ray lasers are not always precise, informing the entire image and producing the result. Some studies have shown that x-ray laser machines often have poor stability in the x-ray imaging properties (Sanchez-Gonzalez et al., 2017). Usually, photons of conventional x-ray machines produce images with energy from 10 to 200 eV. As seen from Appendix C, x-ray lasers might err in approximately 5,6 eV (Sanchez-Gonzalez et al., 2017, p. 4). Thus, the images produced by laser machines may have slight drawbacks inaccuracy of the output. There are many scientific methods to test x-ray lasers, as they have an enormous potential to help discover multiple issues in medicine, physics, biotechnological areas, and even computer technologies.
The Usage of Medical X-rays
Medical imaging creates inner visual structures of the human body for clinical analysis, and medical intervention is required. It is also used to represent human organs and soft tissues (Uzun et al., 2018). Medical imaging enables doctors to look at inner structures of the body covered by skin and bones to prevent and diagnose the disease. In medical imaging, there are two types of x-ray images – these are radiography and fluoroscopy. Even though, nowadays, such methods as computer tomography are promoted widely by medical workers, these two conventional procedures are still relevant.
The process of undergoing medical x-ray imaging is called x-ray radiography. Doctors and medical specialists use it to identify bone fractures, abnormal processes, pneumonia and other lung diseases, foreign objects, and dental issues (NIH, 2021). Moreover, x-rays are used in mammography to detect problems in the breast. Mammography is a medical x-ray imaging method used to prevent, detect, and trace cancer and other breast issues. Mammography methods use low-energy x-rays to generate an image; the projections detect abnormalities (Uzun et al., 2018). The x-ray machine produces an image of soft tissue, and the doctor might see if there is a dense region, which can be potentially dangerous. This thick tissue area may be identified as cancer at the beginning stage; thus, it is crucial to exclude this disease. Indeed, women below 30 are limited to mammography procedures; it is suggested that females from 35 to 40 should undergo mammography screening method once a year (Uzun et al., 2018). Therefore, the x-ray procedures might expose the patient to risk; but it is vital to undergo these investigations to prevent disease development.
Additionally, the usage of x-rays is useful in computed tomography. It is the method that combines both x-rays and computer processing and creates a detailed image of the patient. The computed tomography method transmits x-rays from inner sources to multiple angles to project the image (Uzun et al., 2018). It is also important to note that computed tomography scanners use digital x-ray detectors transmitted to the computer. In addition, computed tomography presents a more detailed image than conventional x-ray medical imaging, as the picture is seen from various angles. Compared with a traditional x-ray machine, computed tomography is mainly used to examine the nervous system, brain, and abdominal organs.
What is more, the method of x-ray radiography is used in fluoroscopy to trace the movement of blood and heart beating. With the x-ray technology, fluoroscopy generates a whole film about the inner structures, which doctors may use to detect diseases and illnesses of organs. It enables them to make a precise diagnosis. Lungs, bones, liver, and other organs are subject to x-ray fluoroscopy. However, patients are subjected to a hefty dose of radiation using this method (Uzun et al., 2018). Therefore, fluoroscopy exposes the patient to a large amount of radiation, which may become dangerous for health.
Angiography is also an examination that uses x-ray radiation; it provides a contrast medium to highlight blood veins and arteries. Indeed, some doctors conduct this procedure through punction; but it can be more dangerous than conventional x-ray therapy. It is usually used to examine arterial and venous supply to various organs, such as the head and upper and lower limbs (Uzun et al., 2018). This method applies to patients if they need to examine and detect various possible issues in the circulatory system.
Therefore, there are many methods of x-ray usage in medical screening. X-rays are used in clinical investigations and are appreciated for simplicity and convenience. Moreover, undergoing x-ray therapy is not painful for the patient; also, it is fast and efficient. Many medical specialists use x-rays instead of other procedures because of the multiple advantages of this procedure. X-rays enable the doctor to examine almost every part of a human’s organism.
COVID-19 and Medical Screening
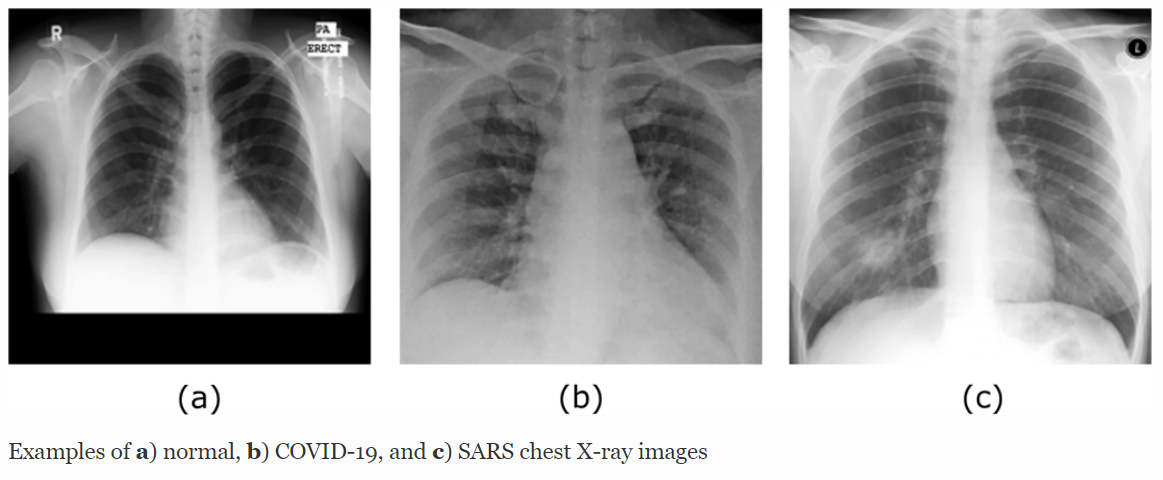
Lung damage and pneumonia caused by coronavirus infection are different from other types of lung diseases. Pneumonia occurs because inflammatory fluid accumulates in the lower respiratory tract, more often against the background of influenza or acute respiratory infections. It is a beneficial environment for the accumulation of bacteria; thus, pneumonia is developing. The sputum itself, which accumulates in the alveoli, interferes with the normal respiratory process. Bacteria settle in it and multiply, which begins to provoke inflammation of individual segments of the lungs. Pneumonia caused by a coronavirus infection is a distinct type of lung damage called pneumonitis (Raghu et al., 2020). It means that interstitial lung tissue, alveolar walls, and nearby vessels can be involved in the pathological process. Thus, inflammatory changes can affect all structures of the lungs. It leads to a violation of gas exchange and normal oxygen saturation of the blood. Appendix A shows differences between normal lungs and those damaged by COVID-19 pneumonia (Abbas et al., 2020). With a coronavirus lesion of the lungs, the radiological image reminds of frosted glass.
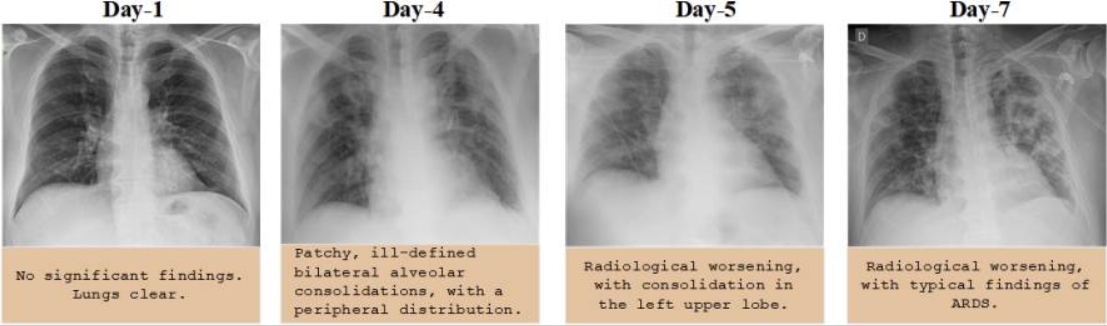
Furthermore, the disease may manifest cowardly, as in the first days, the patient’s lungs are clear, and there do not seem to change significantly. However, as seen from Appendix B, coronavirus pneumonia develops fast; thus, it is crucial to detect it timely (Ozturk et al., 2020). Compared to ordinary bacterial pneumonia, the affected areas look translucent, where the inflammatory process is seen vividly and the tissue structure is dense.
Due to the newly appeared lung disease, COVID-19 doctors hope to use x-rays to diagnose this illness. COVID-19 damages lungs with pneumonia, creating dense mucus within the lungs. The condition requires timely and active checking and medical intervention as it spreads rapidly. The conventional x-ray machine showed a poor result in detecting lung abnormalities. Computed tomography became a more convenient method, as it composes a full 3-d image of the required area; however, the diagnoses are poorly specified and complex to detect (Chan & Li, 2021). Indeed, chest x-rays showed the more accurate result in seeing symptoms of COVID-19 and pneumonia. It is an imaging method that is now commonly used to identify coronavirus and its severe respiratory outcomes (Abbas et al., 2020). The chest x-ray radiology might have multiple advantages over conventional methods of scanning. For example, a chest x-ray is fast; it can analyze several cases simultaneously and is more available than other homogenous tools.
What is more critical, chest x-ray machines can be used in hospitals with limited or absent medical equipment, especially in low-income regions where hospitals do not have an opportunity to provide patients with expensive methods such as computed tomography. It is essential to note that chest radiology imaging systems are available for every medical agency (Khan et al., 2020). Many hospitals are now facing the problem of limited resources in hospitals. For instance, Indian medical agencies have to place patients with COVID-19 outside the hospital, as it is overfilled with infected patients. Some necessary equipment such as modern x-ray machines or computed tomography might be too expensive and unavailable for hospitals. Therefore, a chest x-ray machine is a good solution, as it shows its efficiency and availability for many regions.
There are multiple chest x-rays used nowadays to identify abnormal mucus in a patient’s lungs quickly. Accordingly, this method is more available, cheaper, and more convenient than other methods of lung screening. Besides, one of the advantages of radiography of patients with COVID-19 is mobility. Specialists should use mobile x-ray systems to examine patients with suspected COVID-19. An auxiliary x-ray center with portable equipment is designed for diagnostic imaging of the virus. Specialists can install it closer to intensive care units, which reduces the risk of infection.
Risks of X-rays
Any radiographical device should be used appropriately and controlled by medical specialists. When appropriately used, benefits from x-ray diagnostic are more significant than some possible outcomes (NIH, 2021). These procedures prevent various heart, nervous system, bone diseases, and many other disorders. However, x-rays generate ionizing radiation – a high-energy radioactive substance that potentially may harm the patient’s health. Despite the fact the risk of developing cancer from this radiation is slight, doctors do not recommend undergoing x-ray screenings often. X-ray radiation is an electromagnet radiance located on the scale between ultraviolet and gamma radiation (NIH, 2021). Hence, an x-ray machine is a source of ionizing radiation, and its overdose may lead to severe consequences such as damaging a patient’s DNA. One more issue is that DNA cells cannot confront various negative influences such as radiation from the x-ray source. These cells also might not recover from the impact of x-ray radiance.
It is why the person is recommended not to violate the rules of undergoing x-ray therapies. For example, mutations, genetic changes, and cancer of any organ may become a severe outcome for those who use x-ray often. Moreover, by violating the dose of x-ray radiation, the person risks complicating his existing problems with health (NIH, 2021). Children are sensitive to ionizing radiation produced by the x-ray machine, and thus they have an increased risk for cancer than adult patients (NIH, 2021). Therefore, it is vital to ask the doctor whether the dose of radiation of the x-ray machine is safe for children. Different sources vary in recommending an appropriate amount of x-ray radiation for the patient. For instance, some specialists advise to make a month pause between x-ray therapies; however, the dose is relatively individual for each patient. Indeed, other sources speak that modern x-ray machines are adjusted for safe usage and do not expose patients to the risk of developing various diseases.
Safety Engineering
It is also essential to remember that qualified clinics provide a patient with exceptional medical care, where the doctor writes down all underwent procedures and the history of the diseases. It should contain information about x-ray therapies and the dose of received radiation. If the patient gains a maximal amount, in summary, the person should postpone the treatment to wait a period for undergoing the following procedure. Moreover, the medical specialist who conducts x-ray therapies should possess relevant information about the process. He must know how the machine is generated, adjust the required radiation dose, and warn the patient about consequences. In turn, the patient should tell the specialists about his diseases, underwent therapies and medical contraindications.
Medical specialists use various techniques to prevent the patient from severe consequences of undergoing radiance therapy. For example, the x-ray machine’s tube is placed in a particular protective case, which does not allow x-rays to pass through the patient’s entire body (Shore et al., 2018). The rays are directed to the patient through a particular hole, enabling rays to locate on a targeted area of the body. Moreover, the x-ray tube contains a unique diaphragm installed, which allows the specialist to adjust the dose of radiance.
Accordingly, the patient should be irradiated for as short a period as possible to stay safe and prevent the development of negative consequences. In addition, it is critical to mention that those parts of the body which are not targeted for the x-ray investigation should be covered with a special reflective sheet. It is done to protect other organs from x-ray radiation; especially, it is vital to cover genitals, and the thyroid gland as these parts are sensitive to radiance. Violation of this rule may lead to damaging healthy organs and result in high-cost treatment.
It is also essential to note that medical specialists who conduct x-ray procedures should know how to make a relevant report. The medical piece is vital in radiology practice for generating and evaluating radiographs or radiological images (Syeda-Mahmood et al., 2020). The task of the medical specialist is not limited to providing the procedure but also to making appropriate conclusions for the diagnosis (Syeda-Mahmood et al., 2020). For the clinical specialist or doctor providing the patient with an x-ray therapy, it is essential to write down all findings detected during the radiography investigation. For instance, the specialists should find and record problems encountered in the patient’s part of the body or tissue. Furthermore, if the specialist sees other issues out of his area of investigational responsibility, he should write them down in the record. All radiologists are taught to simultaneously identify radiological findings and write them in the patient’s medical history in an inappropriate way.
Likewise, if the patient comes to the chest x-ray to detect lung problems, the doctor will record other identified disturbing findings. It is done to improve the medical communication between the patient and clinical organizations. Moreover, it may save patients’ time and enables them not to wait till the subsequent investigation. What is more, the clinical specialist should record his impressions according to his medical background. For example, if the patient has pneumonia, he is recommended to visit the therapist to receive appropriate treatment. Therefore, the medical radiography specialist may redirect the patient to another doctor to identify and cure other health issues.
Conclusion
Overall, x-ray therapy helps identify various diseases and health issues. The x-ray machine is a conventional method for undergoing radiography procedures, and it is used in different medical areas. Many doctors use this tool for dental, chest, brain, and vessel investigations. Moreover, the x-ray method plays a significant role in medical imaging due to its ability to trace and prevent health issues. It is a convenient, painless, fast, and relatively cheap method for medical procedures. Nowadays, x-ray methods are used to detect coronavirus pneumonia and other related lung issues, enabling doctors to prevent the adverse outcomes of the disease. Indeed, medical workers often do not appreciate undergoing x-ray therapies because of ionizing radiation that can damage DNA and a patient’s healthy organs. It is also essential to mention that radiography specialists who work with x-ray devices are trained to record all possible findings to improve health care communication.
References
Abbas, A., Abdelsamea, M. M., & Gaber, M. M. (2020). Classification of COVID-19 in chest x-ray images using DeTraC deep convolutional neural network. Applied Intelligence, 51(2), 854–864. Web.
Chan, J. H., & Li, C. (2021). Learning from imbalanced COVID-19 chest x-ray (CXR) medical imaging data. Methods, 1, 1-9. Web.
Concerning Reality. (2019). How do x-rays work? [Video]. Web.
Khan, A. I., Shah, J. L., & Bhat, M. M. (2020). CoroNet: A deep neural network for detection and diagnosis of COVID-19 from chest x-ray images. Computer Methods and Programs in Biomedicine, 196, 105-108. Web.
NIH. (2021). X-rays. National Institute of Biomedical Imaging and Bioengineering. Web.
Ozturk, T., Talo, M., Yildirim, E. A., Baloglu, U. B., Yildirim, O., & Rajendra Acharya, U. (2020). Automated detection of COVID-19 cases using deep neural networks with X-ray images. Computers in Biology and Medicine, 121, 1-10. Web.
Raghu, G., Remy-Jardin, M., Ryerson, C. J., Myers, J. L., Kreuter, M., Vasakova, M., Bargagli, E., Chung, J. H., Collins, B. F., Bendstrup, E., Chami, H. A., Chua, A. T., Corte, T. J., Dalphin, J. C., Danoff, S. K., Diaz-Mendoza, J., Duggal, A., Egashira, R., Ewing, T.,… Wilson, K. C. (2020). Diagnosis of hypersensitivity pneumonitis in adults. An official ATS/JRS/ALAT clinical practice guideline. American Journal of Respiratory and Critical Care Medicine, 202(3), 36–69. Web.
Sanchez-Gonzalez, A., Micaelli, P., Olivier, C., Barillot, T. R., Ilchen, M., Lutman, A. A., Marinelli, A., Maxwell, T., Achner, A., Agåker, M., Berrah, N., Bostedt, C., Bozek, J. D., Buck, J., Bucksbaum, P. H., Montero, S. C., Cooper, B., Cryan, J. P., Dong, M.,… Marangos, J. P. (2017). Accurate prediction of X-ray pulse properties from a free-electron laser using machine learning. Nature Communications, 8(1), 1-11. Web.
Shore, R. E., Beck, H. L., Boice, J. D., Caffrey, E. A., Davis, S., Grogan, H. A., Mettler, F. A., Preston, R. J., Till, J. E., Wakeford, R., Walsh, L., & Dauer, L. T. (2018). Implications of recent epidemiologic studies for the linear nonthreshold model and radiation protection. Journal of Radiological Protection, 38(3), 1217–1233. Web.
Syeda-Mahmood, T., Wong, K. C. L., Gur, Y., Wu, J. T., Jadhav, A., Kashyap, S., Karargyris, A., Pillai, A., Sharma, A., Syed, A. B., Boyko, O., & Moradi, M. (2020). Chest x-ray report generation through fine-grained label learning. Medical Image Computing and Computer Assisted Intervention – MICCAI 2020, 1, 561–571. Web.
Uzun, D., Uzun, B., Sani, M., & Ozsahin, I. (2018). Evaluating x-ray based medical imaging devices with fuzzy preference ranking organization method for enrichment evaluations. International Journal of Advanced Computer Science and Applications, 9(3), 110-245. Web.
Appendix A
Lungs Damaged by COVID-19
Appendix B
The Development of COVID-19 Infection in the Lungs
Appendix C
Photon energy of the x-ray laser radiation