Abstract
The research is aimed at investigating how the surgical personnel in ambulatory surgical centers in the northeastern part of the United States who learn new, advanced medical-surgical technology through in-services and the acquired level of skill competency perceive their skill level or competency with medical-surgical technology following training. The research questions addressed in the dissertation include: How do surgical personnel describe their experience of learning new, advanced medical-surgical technology through in-services at ambulatory surgical centers in the northeastern United States? How do surgical personnel at selected ambulatory surgical centers experience in-services as a means to learn to use new, advanced medical-surgical technology? How do surgical personnel describe the effect of learning new, advanced medical-surgical technology through in-services with respect to their self-described confidence in their skill? The qualitative descriptive design was used to systematize, analyze, and interpret the data collected via questionnaires from 13 surgical room personnel members. The results of the study demonstrate that the most frequent shortcomings of in-service and on-the-job training include inappropriate methodology and curriculum, the lack of follow-up activities, insufficient motivation, ineffective trainers, team disturbances, rushed training, and low productivity. Despite the shortcomings, 85% agreed that on-the-job training is an effective way of learning new skills required to use advanced surgical technologies. Practitioners and leaders in the field of surgical technology training are encouraged to construct better training sessions, employ more qualified experts and trainers, and allocate sufficient time and resources for continuous learning.
Introduction
During calendar year 2016, there were 48.3 million surgical and nonsurgical procedures performed across the United States in hospital operating rooms and ambulatory surgical centers (Hall, Schwartzman, Zhang, & Liu, 2017). An average of one out of 25 people was admitted for surgery of some type annually. Surgeons, anesthesiologists, certified registered nurse anesthetists (CRNAs), surgical technologists, and patients have relied upon medical technological advancements. The focus of this study was to learn the attitudes and experiences of surgeons and staff regarding the training and education in advanced surgical technology.
Scholars and practitioners have spoken of the need and value of such technology as it has improved operating room efficiency (Deutsch et al., 2015), quality of health care outcomes (Ekkelenkamp, Koch, de Man, & Kuipers, 2016), surgical staff job satisfaction (Acton, 2013a), and patient safety and satisfaction (Champagne, 2013). In contrast, multifactorial causes behind operating room medical technology are not meeting the needs of healthcare providers and patients (WHO, 2010). Among these causes is one cause that can be attributed to the lack of working knowledge of operating room medical technology, procedural skill(s), or procedurally based competency (Moore et al., 2015).
A deficiency in learning curves (Acton, 2013b; Deutsch et al., 2015; Jaffe et al., 2017; Moore et al., 2015; Panait, Shetty, Shewokis, & Sanchez, 2014; Romeo, 2016; Stanford, Lee, Masaquel, & Lee, 2015), among other reasons, contributes to a lack of advanced education and training in operating room medical technology (Gallagher et al., 2014; Roberts, Bell, & Duffy, 2006). Learning the mindset of surgeons and surgical staff toward new surgical technologies that require different skill sets than the traditional open form of surgery would help with training and in-service procedures.
A compromised quality of care, in conjunction with less efficiency in care and subsequent decrease in patient satisfaction because of lengthy learning curves, affects the perception of learners (McLaughlin, 2012). Especially significant are the beliefs and attitudes surgeons and staff hold regarding strategies, methods, and tools for advanced technological training and education, which comprise the topic of this study. Surgeon and staff competency with new surgical technologies must be maintained to take full advantage of the value of such technologies. Knowledgeable, skilled, and competent operating room staff should be willing to try, use, and even recommend or approve new technologies (World Health Organization, 2010). In this way, the staff would make proper and innovative use of the new surgical support technologies.
The remaining sections of Chapter 1 include the background of the study, the problem statement, the purpose statement, and the research questions serving as guides for the development of the study. The discussion on processes of data analysis sets the foundation for the rest of the study. Chapter 1 also includes discussions on the nature of the study and practices relative to the privacy and confidentiality of both the participants and the data.
Background of the Problem
Historically, performing surgeons had to demonstrate procedural competence continually evolving experience, domain knowledge, landmark knowledge (recognition and recall about the anatomy), and conventional procedural knowledge and a willingness to share that knowledge (Dubé & Rostom, 2016; Jang, Ko, Choi, & Kim, 2017; McLaughlin, 2012; Sharma, Surek, Stewart, Stephens, & Wright, 2016; Sood et al., 2015; WHO, 2010). Surgical staff must engage in such practices to achieve efficiency and maintain patient safety by using standardized, anticipatory knowledge regarding operating room preparation procedure, set-up, patient preparation, the surgical procedure, and patient recovery plans (McLaughlin, 2012).
The Accreditation Council of Graduate Medical Education endorsed six core competences that every physician should demonstrate patient care, medical knowledge, practice-based learning and improvement, interpersonal communication skills, professionalism, and systems-based practice (Roberts et al., 2006). To meet Accreditation Council of Graduate Medical Education requirements, educators need to include surgical education necessary to support the knowledge, skills, and practice in the operating room surgical center.
Traditional surgical education consisted of self-directed study, didactic learning, simulation or cadaver laboratories, and scrubbing in cases performed by an expert or under the supervision of a proctor or mentor (Jaffe et al., 2017). Advanced surgical technologies require not only the continued need for knowledge and knowledge sharing but also a need for shared purpose (Dubé & Rostom, 2016) and shared workload (Entezami, Franzblau, & Chung, 2012). When individuals with different learning curves are involved, different surgical innovations are necessary (WHO, 2010). including using supportive ways to meet the needs of individuals
With advances in surgical technologies, such as minimally invasive surgical procedures including colonoscopies, endoscopies, laparoscopies, and laser surgery, steeper or more significant learning curves require additional or different training approaches to meet the needs of operating room staff. The learning curve is the time and number of repetitions required to achieve an acceptable (proficient) outcome of the given task (Moore et al., 2015; Sood et al., 2015; WHO, 2010).
Education and training required for surgical technological advancements have also had to advance to shorten or support steep learning curves to maintain efficiency and patient safety at the same time. Such education includes training devices for surgeons to use robotic operating systems, surgical simulators such as box trainers for laparoscopic surgery, animal models, virtual reality surgical simulators, and full procedural simulators. One such simulator is the epiduroscopy training simulator for spatial cognition learning as well as ultrasound-assisted surgery and color Doppler-guided surgery (Alfredson & Isaksson, 2014; Harrysson, Hull, Sevdalis, Darzi, & Aggarwal, 2014; Jang et al., 2017; Moore et al., 2015; Panait et al., 2014; Stefanidis, Scerbo, Montero, & Smith, 2012).
Such surgical technology training and supports might maximize the efficiency of surgical procedures and assure or improve patient safety and satisfaction. Much research is available on the need for ongoing education, but no studies were found on the experience of surgical staff attending trainings and in-services (Deutsch et al., 2015; Jaffe et al., 2017; Romeo, 2016; Stanford et al., 2015). The focus of this study was on learning how surgeons and surgical staff members perceive in-services used as training in the use of advanced technology used in surgery.
Educational Benefits of Surgical Training Programs
The advancement in surgical technology, such as robotically assisted surgical devices, has necessitated new measures of surgical competency that allow physicians to be evaluated for preparedness in evolving operating room environments. In general, surgical training programs have been demonstrated to mitigate learning curves for surgeons using both nonrobotically assisted and robotically assisted surgical technologies. The emergence of global surgery has led to the development of residency programs that integrate international surgical knowledge into students’ training, particularly with regard to settings with poor resources (Swain et al., 2015). A lack of knowledge about types of training remains the most effective for both scenarios.
In traditional (i.e. non-robotic) surgical training, adequate training programs have been shown to help trainees meet and exceed different evaluative metrics such as laparoscopic knot-tying performance (Chang, Satava, Pellegrini, & Sinanan, 2003). Surgical training programs, as stated, are designed to acclimate surgical residents with the practice of procedures and operations under the guidance of a supervising surgeon (Nemani et al., 2018). The objective is for these supervisors to measure the skills of the residents to determine their level of competency (Nemani et al., 2018).
In particular, Molinas, Binda, Sisa, and Campo (2017) found that psychomotor training could improve learning times with respect to the learning curve of laparoscopic intra-corporeal knot tying. Because the supervisors’ assessment of the students’ performance can be subjective in nature, the McGill Inanimate System for Training and Evaluation of Laparoscopic Skills (MISTELS) was created as a means to measure laparoscopic surgical skills (Nemani et al., 2018). The earlier students were exposed to surgical training programs, the greater their confidence in undergoing surgical training and the greater the results of the training (Karmali, 2017; Sharma et al., 2016).
Similarly, the more years of training residents undergo, the greater the quality of the residents’ performance (Williams et al., 2017). The greater the quality, according to Williams et al. (2017), the more autonomy is ultimately afforded to these surgeons. This was further confirmed by a study of 27 supervising surgeons who assessed 1,490 operations under the scope of 127 unique procedures that were completed by 31 residents (Williams et al., 2017).
Training programs have also been shown to be effective in robotic-assisted surgical training, although more formalized and universal approaches have still yet to be adopted. According to Sridhar, Briggs, Kelly, and Nathan (2017), residents must first undergo formal training that provides instructions based on skill acquisition and safety measures prior to conducting the procedures independently. This is particularly relevant, because the incidence of robotic surgery has increased exponentially over the past 10 years, with more than 650,000 performed worldwide in 2015 (Aridhar et al., 2017). Specifically, more than 1.5 million procedures have been performed utilizing the da Vinci Surgical System–a specific surgical robot used to make minimal incisions–as of 2015 (Fisher et al., 2015). The training process for robotic surgery can be divided into two components: patient-side training and console training (Aridhar et al., 2017). Patient-side training is the first aspect surgeons must learn during their residency.
Patient-side training introduces the resident to the surgical process, while facilitating the succession of skills that are unique to the resident (Aridhar et al., 2017). Through this process, the resident understands how to operate the robotic arms (Aridhar et al., 2017). Console training is the interface that essentially dictates the movement of the robotic arms, which can be learned via online courses (Aridhar et al., 2017). Despite the scholarship available about training and credentialing for robotic surgery in certain fields, it has yet to be standardized (Gross et al., 2016).
No single curriculum outlines the teaching of robotic surgical technologies, deeming the learning process as largely unstructured (Fisher et al., 2015). Similarly, this lack of consistency extends into the health care setting with requirements for resident surgeons varying from hospital to hospital and institution to institution (Fisher et al., 2015). The unified theory of acceptance and use of technology showed the three main barriers to adoption of robotic-assisted surgery for both users and nonusers were perceived ease of use and complexity, perceived usefulness, and perceived behavioral control (Benmessaoud, Kharrazi, & MacDorman, 2011).
Another factor hindering the development of training programs has been the slowness with which robotic technologies are incorporated in curricula. This slowness is also the result of lack of clear-cut curricula concerning robotic surgical tools (Fisher et al., 2015). Because no standardized outline of curricula relating to robotic technology in surgery exists, no standardized means to measure performance exist. Although most surgical residents have robotically assisted surgical technology at their institution and have participated in robotic surgical cases, few residents received formal training before participating in a robotic case (Farivar, Flannagan, & Leitman, 2015). Most residents believe training on robotic technology is important.
A successful robotically assisted training curriculum must be based on didactic learning, reading, bedside training, simulation, and training in the operating room (Winder et al., 2016). A concern is that as the health care industry and, consequently, surgical measures continue to progress and evolve, the industry is tasked with remaining up-to-date (Rogula, Acquafresca, & Bazan, 2015). This industry has the responsibility to provide ongoing training and education for its residents and professionals alike (Rogula et al., 2015), which can be both time-consuming and costly.
Further complicating the development of training programs for robotic-assisted surgical training has been a general disagreement about the benefits of surgical robots to operating room procedures. Robotic training in general surgical residency does not amount to extra operating room time (Honaker, Paton, Stefanidis, & Schiffern, 2015), Complex surgical robotic equipment increases opportunities for technological failures, increases communication requirements for the whole team, and can reduce the ability to maintain vision in the operative field (Catchpole et al., 2016). Covens et al. (2016) argued that robots provide no measurable benefits to learning curves in surgical training. While robot costs are higher, the health outcomes are comparable.
Smyth, Deveney, and Sade (2013) stated that the surgical robot actually decreased the learning curve for experienced surgeons. This learning curve decreased so much so that by the seventh time the surgery was performed, the operation time involving the robot was faster than surgeries performed by surgeons who had previously completed 1,000 traditional laparoscopic surgeries (Smyth et al., 2013). On the contrary, Bach, Miernik and Schnthaler (2014) reported a lack of a straightforward understanding of a sufficient learning curve for robot-assisted laparoscopic surgery for prostatectomy and upper tract procedures.
The researchers stated that a clearer understanding of how to bolster the educational process might substantially affect the development of the surgical resident (Bach et al., 2014). Einarsson (2014) adamantly declared that robotic surgery does not provide any benefits to the patient when compared with traditional laparoscopic surgery. Einarsson also affirmed that the complexity of the new technology lengthens the learning curve for professionals because of the need to understand how to manipulate the technology and successfully utilize its range of capabilities. Consequently, the researcher claimed that no evidence exists that indicates robotically assisted surgery decreases the time period of a surgery or improve the safety measures of the surgery (Einarsson, 2014). Considering the varying perspectives of the aforementioned researchers, ambiguity surrounds the notion of whether robotic-assisted surgery provides the health care industry with positive, negative, or null results.
Problem Statement
Advancement of medical and surgical technologies brought the need for more effective training and education to achieve competency for surgical staff. The research problem involves a lack of understanding the experience of surgical personnel attending in-services to learn new, advanced medical-surgical technology (Jaffe et al., 2017; Romeo, 2016). The deficiency exists due to learning curves (Acton, 2013b; Deutsch et al., 2015; Jaffe et al., 2017; Moore et al., 2015; Panait et al., 2014; Romeo, 2016; Stanford et al., 2015), and among other reasons, the delivery pattern used to train staff in surgical medical technology (Gallagher et al., 2014).
Some researchers have determined that less than half (36%) of endoscopy trainees self-reported their skill level as proficient (Stanford et al., 2015). Inexperienced trainees may perform more than 180 procedures before they can be considered competent (Ekkelenkamp et al., 2016). New surgical technologies require different skill sets than traditional open surgery once required (Stanford et al., 2015). Learning new skills and becoming competent with advanced technology is a necessary part of surgical success.
Much research on the competencies of surgical staff exists. Yet no specific research into the most effective education and training to accommodate different learning curves to achieve surgical competency using new surgical technologies (Ekkelenkamp et al., 2016) is available. Researchers should determine which types of education and training are most effective in achieving surgical staff competencies with new surgical support technologies. Maintaining a standard of excellence for graduating surgical residents requires a comprehensive and consistent pattern of surgical education (Champagne, 2013). The same expectation applies to achieving and sustaining competency, efficiency, and knowledge-sharing efforts for all surgical staff using advanced surgical technologies.
Purpose of the Study
The purpose of the qualitative descriptive study is to understand the experience of surgical personnel in ambulatory surgical centers in the northeastern part of the United States who learn new, advanced medical-surgical technology through in-services and the acquired level of skill competency. The aim is to learn how surgical personnel perceive their skill level or competency with medical-surgical technology following this type of training. At this stage in the research, the training approach would generally be defined as Operating Room Training.
The need for training and education for advanced surgical technologies is yet to be closely investigated in terms of how the education is most effective for hospital efficiency (Alfredson & Isaksson, 2014; Deutsch et al., 2015; McLaughlin, 2012), improved quality of health care outcomes (Ekkelenkamp et al., 2016; McLaughlin, 2012; Moriates, Dohan, Spetz, & Sawaya, 2015; Phillips, 2013), enhanced surgical staff job satisfaction (Acton, 2013a; McLaughlin, 2012), and increased patient safety and satisfaction (Champagne, 2013; Deutsch et al., 2015; El Bardissi & Sundt, 2012; McLaughlin, 2012).
The question remains concerning why operating room medical technology is not meeting the needs of healthcare providers and patients (WHO, 2010). One possible answer is a lack of operating room working knowledge and procedural skill(s)—or procedurally based competency—with medical technology and deficiency resulting from lengthy learning curves (Acton, 2013b; Deutsch et al., 2015; Jaffe et al., 2017; Moore et al., 2015; Panait et al., 2014; Romeo, 2016; Stanford et al., 2015). A lack of or insufficient advanced operating room medical technology education or training would have seriously negative results. (Gallagher et al., 2014; Roberts et al., 2006). Because a compromise in the quality outcome of care might occur in conjunction with less efficiency of care and negatively impacted provider and patient satisfaction, this study is intended to how in-service training and education for surgeon and staff competency with new surgical technologies.
The process involved a sample population of surgical staff sharing their experiences and perceptions with operating room competency following the in-services or training on new medical-surgical technologies. The study results should lead to clearer understanding, from the perspectives of operating room staff, on how different education/training modalities prepare staff to use new technologies in actual practice in the operating room. Based upon an analysis of the shared experiences and perceptions, the insights gained from the responses could be used to improve hospital education/training practices.
Few, if any, researchers to date have focused on training from the perspective of the learners, preferring to research the use of the advanced equipment in the operating room in specific surgical procedures (Ekkelenkamp et al., 2016). Because quantitative studies and mixed studies focused as specific factors on the implementation of medical-surgical technologies, a plethora of information on training and use of advanced technologies is available. This study was designed to shed light on the means of enhancing knowledge and skill acquisition regarding the use of modern technology by surgeons and the operating room team as well as on the hazards that may appear (Matern & Koneczny, 2007, p. 1965).
By combining qualitative and quantitative methods to attain results that are more comprehensive, the affective nature of the training would be clearer. If a mixed method is used, the research may help leaders develop “a strong motivation” among the staff when training staff on using new surgical technology (Christensen, 2013, p. 251). The research results could be used to inform policy and practices in attempts to facilitate rapid improvement in the use of new equipment, the application of nontechnical skills, the success of surgeries (Gordon et al., 2012, p. 1042), and the satisfaction and safety of all.
Population and Sample
This descriptive study involved the population directly responsible for surgical care in accredited hospitals and surgical units. The general population included surgeons, anesthesiologists, CRNAs, and surgical technologists working in the northeastern United States. The number of operating personnel working in the operating rooms in the selected area was unknown. However, on average, a surgical team working in an operating room normally consists of 10 to twelve members including specialists and their leaders (Arakelian et al., 2011). Based on these data, the estimated number of participants was set at 10 to obtain a manageable number of responses. The importance of working with surgical staff who use advanced technological surgical equipment was vital to a credible study. Small samples are suitable for qualitative studies because the sample represents a particular and in-depth perspective of the topic (Smith, J. et al., 2009). The sample consisted of a total of 10 participants who met the criteria for inclusion in the research.
Inclusion criteria governing participation in the study follow: (a) Participants in this study had experience working in the surgical center and (b) had attended in-services on new technologies by at least two different modalities (c) within the last two to three years. The researcher attempted to ensure that (d) participants had experience with in-person/team-based training as well as technologically mediated training. In that way, (e) the participants can speak meaningfully about the advantages and disadvantages of either a face-to-face training or a technology-based form of delivery.
Significance of the Study
The theoretical basis for this study is Knowles’ (2015) theory of andragogy. While articulating the needs of adult learners, Knowles was one of the first to discuss the factors influencing adult education in its many forms. This study may be the first to apply Knowles’ theory to teaching advanced technology in the field of surgery, expanding a theory written for adults in general. The use of an androgenous approach in this study enhanced the number of applications documented for the theory.
This study may add clarifying insights into the learning experience. The results of this study might also provide the insights necessary to develop guidelines for curriculum development for medical training or educational efforts to assist surgeons and operating room personnel in maintaining competency with advanced technology. Given knowledge of the responses of operating room personnel and surgeons, yielding information on their perceptions and experiences of different forms of educational delivery might be obtained.
Numerous researchers examined the effectiveness of training in the operating room or on “the value of delivering a theater induction curriculum” (Patel, Aggarwal, Osinibi, & Darzi, 2012, p. 266). Yet studies that focused on training in the use of the advanced equipment in the operating room in specific surgical procedures were less available (Ekkelenkamp et al., 2016). The current study narrowed the gap in the body of knowledge by extending the understanding of the experiences of operating room personnel regarding continual learning of new technology.
This study also shed light on the means of enhancing knowledge and skill as well as the hazards that may appear (Matern & Koneczny, 2007, p. 1965). The responses of the surgeons and the operating room team provided the meaning of training in advanced surgical technology for those who have experienced both types of training: in-service and digital training. The findings from this descriptive study would lead to a clearer understanding of the most efficient and effective means of training operating room personnel. The research might also help leaders develop “a strong motivation” among the staff to use new technology (Christensen, 2013, p. 251). Gordon, Darbyshire, and Baker (2012) also expected a rapid improvement in the use of new equipment and nontechnical skills as well as in the success of surgeries.
Nature of the Study
The qualitative descriptive design was conducted with a focus on context and interpretation in terms of how and why (Patton & Cochran, 2002; Rossman & Rallis, 2003), whereas a quantitative research design presents results in quantities. An in-depth description of experiences is needed to learn the most accessible and most effective training approaches for operating room staff competency with new medical-surgical technologies; thus, qualitative methods are most appropriate for the study. With the more open intuitive approach of a descriptive design, a researcher can learn the attitudes, intentions, and experience of the participants. One purpose of a descriptive design is to learn how individuals experience a phenomenon (Yin, 2017) to prepare the way for additional research on that phenomenon.
For the purpose of this study, the use of a qualitative descriptive design opens the focus of the study (Patton & Cochran, 2002) to the surgical staff. Other designs, such as ethnography, which researchers use to study the culture of a group and its traditions and its mores, requires researchers to immerse themselves within the culture (Rossman & Rallis, 2003). Another qualitative design is grounded theory, used to generate a theory from data collected in order to develop a theory or add to an existing theory (Rossman & Rallis, 2003). Education and training are both well-researched areas, and the purpose of this study would not add new substance to educational field but would add insights in a new application to the literature. Using a qualitative descriptive design to learn how surgeons and surgical staff experience education and training in advanced technological surgery is the most appropriate qualitative design for this study.
A sample of 10 surgeons, anesthesiologists, CRNAs, and surgical technologists were selected from the population of professionals responding from northeastern United States. Participants had working experience in the surgical center and had attended in-services on new technologies by means of at least two different modalities within the last two or three years. Participants should also have had experience with some form of in-person/team-based training as well as some form of technologically mediated training. They could speak to the pros and cons of different forms of learning with a relevant basis for comparison.
Through responses to the questionnaire by the participants, the researcher was able to collect descriptions to be analyzed using the thematic analysis approach outlined by Braun and Clarke (2012). Responses to the questionnaire yielded insights into the experiences of surgical staff regarding education leading toward efficiency and competency needed for patient safety and satisfaction. Potential solutions for the problem of education and training using advanced surgical technology surface to meet these requirements. The written data provided a well-rounded context for interpreting each participant’s data.
The use of Braun and Clarke’s (2012) thematic analysis help to identify and describe these themes relative to surgical competence, operating room efficiency, and patient safety and satisfaction. The data source included descriptions by surgical staff trained and educated in proper advanced surgical technology delivered through different forms of training. In this study, the data took on meaning when considering the theory of adult education developed by Knowles (2015). The theoretical foundation underlying this study, Knowles’ theory of andragogy served as a guide by which to evaluate the presentation of new information.
Research Questions
As the driving force of the objectives of the study or specific elements of the issue under analysis, the use of research questions to guide the development of the study allows for rational analysis (Eshun & Eshun, 2013). The aim of this study is to learn the experiences of surgical staff in the use of advanced surgical technologies in terms of settings and frequency of use. This study is also intended to describe staff willingness to use, staff use knowledge and skill as they contribute to operating room efficiency, staff knowledge-sharing willingness, staff job satisfaction, patient safety, and patient satisfaction. Also, under investigation were the participants’ overall commitment to contribute to the development of the healthcare facility through the improvement of technology-associated policies and procedures. The research questions of the present study are as follows:
- RQ 1: How do surgical personnel describe their experience of learning new, advanced medical-surgical technology through in-services at ambulatory surgical centers in northeastern United States?
- RQ 2: How do surgical personnel at selected ambulatory surgical centers experience in-services as a means to learn to use new, advanced medical-surgical technology?
- RQ 3: How do surgical personnel describe the effect of learning new, advanced medical-surgical technology through in-services with respect to their self-described confidence in their skill?
Theoretical Framework
The theoretical basis for this study is Knowles’ (2015) theory of andragogy. As adult education became more widespread in the 1980s in the United States, Knowles articulated the differences between teaching children and teaching adults. While Knowles was one of the first to discuss the factors influencing adult education, theorists and practitioners have extended or refined the theory of andragogy to reflect the many forms of delivery found in adult education.
Applying the theory to the present study aids in understanding how surgical staff are experiencing surgical education to increase comprehension and skill in the use of advanced technological instrumentation in the operating room. The research problem is a lack of understanding the experience of surgical personnel in ambulatory surgical centers in the northeastern United States attending in-services to learn new medical-surgical technology. In-services can take many forms from seminars and workshops to on-the-job training. Whatever the form of training, the principles of andragogy apply. To conduct this study, the researcher needed to consider and address a multidimensional paradigm and gather descriptions from a sample of surgeons and surgical staff. This framework is based on Knowles’ (2015) theory of andragogy.
Overzealous focus on efficiency has been criticized for its McDonaldization of surgery and surgeons (Waring & Bishop, 2015). Taken into partial consideration, scientific medicine in America and Europe formerly “exemplifying a comparable will to control and standardise [sic] practitioners and patients ” (Whitfield, 2015, p. 421). As health care became subject to statements of profit and loss, surgery and efficiency have been associated with the principles of standardization and specialization (McLaughlin, 2012; Whitfield, 2015). Surgical procedures were standardized (or efforts were made toward standardization) when involving medical technologies to be mastered, especially those with a steep learning curve.
For efficiency as well as for competency, members of the surgical staff learning and using advanced medical and surgical technologies must have domain, landmark, and procedural knowledge and skills. This knowledge and skill requirement depends upon surgical education, to which Knowles’ (2015) andragogy lends itself (Aho et al., 2015; GearhartWang, Gilson, Chen, & Kern, 2012; Knowles, Holton, & Swanson, 2005; Merriam, 2001; Merriam, Caffarella, & Baumgartner, 2012; Ozuah, 2016).
According to Knowles (2015), the assumptions of pedagogy—i.e., that learning is teacher-directed, include the belief that learners are dependent. A learner’s prior experience is not a factor to learning (Merriam et al., 2007)—contrasted with the assumptions of adult learning. Knowles-based andragogy involves a set of assumptions that includes (a) learning is student-centered, (b) learners display independent characteristics and are self-directed, (c) a learner’s experience is crucial to learning, and (d) learners are motivated by intrinsic (internal) factors (Merriam et al., 2007; Ozuah, 2016). Surgeons and surgical staff using advanced surgical and medical technologies should learn from educators using equally advanced methods of education. The concepts of andragogy also need to be integrated into surgical education for effective knowledge and training.
Definition of Terms
The following operational definitions are used interchangeably throughout the study:
Andragogy: The sibling philosophy (and practice) to pedagogy, andragogy is the philosophy and practice of teaching and learning for adults (Knowles, 2015).
Competence/competency: Competence was and to some extent still is defined by the achievement of a specified number of procedures as determined, measured, and assessed by experts (Dubé & Rostom, 2016; Tassios et al., 1999).
Effective: While effective is a highly subjective adjective, a procedure is considered effective when it results in the intended optimum outcome—when it is efficient, safe, and satisfactory for both surgical staff and patients (Tomlin, Humphrey, & Rogers, 1999).
Efficiency: Efficiency in surgical contexts involves the extent to which the work performed is most useful and least wasteful given the time spent and the effort extended (Alfredson & Isaksson, 2014; Deutsch et al., 2015; McLaughlin, 2012
Learning curve: The learning curve is the time and number of repetitions required to achieve an acceptable (proficient) outcome of the given task (Moore et al., 2015; Sood et al., 2015; WHO, 2010).
Assumptions, Scope, Limitations, and Delimitations
Every research study involves a scope indicating what is and is not covered in the study. Another element found in research involves the limitations. The limitations refer to those situations and conditions that the researcher controls, necessitating certain requirements. Also, assumptions pertaining to the study provide clarity of the ideas and principles that are perceived by the researcher in a way that predetermines the direction of the study. Potential delimitations did not interfere or hamper the study in any way.
Assumptions
This study entails both general and specific assumptions. The first assumption deals with the requirements of education and training for all surgical staff. A second assumption is that learning curve amelioration can be attempted by measures used by the subjects and the supervising experts.
First, an assumed is that some forms advanced surgical technology education and training are better in terms of quality and efficacy produced than other advanced surgical technology education and training. For example, several authorities (e.g., Smith, R. D., 2009) have criticized didactic learning in isolation as the result of didactic teaching methods. Didactic teaching includes the assumption that where insufficient education and training persists, recommendations can be made for more effective patient care, patient safety, and patient satisfaction. The result includes standardization and structuring (Ration) to adopt, use, and share knowledge on new surgical technologies.
A second assumption is that learning curve amelioration measures used by the subjects (and the supervising experts in their domain: if the measure for lessened learning curves is decreased number of repetitions of a procedure before competency is achieved, the researcher will take on that measure and criterion to discuss learning curves and education to remediate them. If the measure of learning curves is based on a subjective expert-determined demonstration of skills, knowledge, or expertise, the discussion of learning curve remediation will include evaluation of that measure. This follows the assumption by Ekkelenkamp et al. (2016) that competence is often measured on an individual basis and depends upon the particular procedure being performed.
Scope
The scope of the study was by no means comprehensive and was intended to describe the experience of surgical staff learning how to use advanced surgical technologies proficiently. The types of surgical procedures and new surgical technologies are great in number, and it was not possible to specify or narrow the scope of this study to just one technological advancement. The scope did not center on the content of the in-service; rather, the focus of the study was on the perceptions of delivery methods of learning.
Limitations
A few limitations surfaced in this study. One limitation was the number of participants available when the very nature of their work keeps them engaged in efforts that involve prohibitive schedules. The aim was to allow enough time and flexibility to accommodate each participant’s schedule. Another limitation was the diversity of the surgical staff members, whereby experience on the part of each staff member would not be commensurate in terms of training aptitude, and the heterogeneity of the sample population may be limited, but in this case, was not.
The research was conducted with surgeons, anesthesiologists, CRNAs, and surgical technologists to gain their perceptions of training approaches used in ambulatory surgical centers located in the northeastern United States. The third limitation involved the subjective nature of perceptions by participants in varied roles with differences in experience and types of involvement with the technologies and training. Participants shared their perceptions and experiences, and such variety in the sample served to inform the research with a contextual richness that a strictly homogeneous group might not provide. The potential delimitations did not interfere or hamper the study in any way.
Delimitations
In this study, delimitations that might have hindered the collection of data and process of analysis did not occur. Despite the serious conditions arising from the spread of COVID-19 throughout the world and especially in the northeastern United States, the surgical staff at the hospital continued their normal routines. That is, they continued as best they could, so the at least, until the data collection was completed.
Chapter Summary
To summarize, Chapter 1 included an overview of the issues surrounding the ongoing training needed by operating room personnel and surgeons to achieve efficiency and protect patient safety by using anticipatory knowledge regarding operating room preparation procedure, set-up, the surgical procedures, and patient recovery plans (McLaughlin, 2012). The qualitative descriptive study contained the main elements of a study on the perceptions and experience of operating room staff when training to learn to use advanced medical-surgical technologies.
Scarce information was found on the learners’ experience with on-the-job training, specifically in-services, a form commonly used in the fields of health care and education (Ekkelenkamp et al., 2016). Encouraging an environment based on the need for proficient skills and a willing attitude will enhance a welcoming attitude toward new technologies in the surgical care of patients. Chapter 2 contains a review of the literature currently available on the subject. The sources were reviewed to learn the work that precedes this study and to add to the body of knowledge on the subject of the study.
Literature Review
The purpose of the qualitative descriptive study is to understand the experience of surgical personnel in ambulatory surgical centers in northeastern United States who learn new, advanced medical-surgical technology through in-services. The research problem is that there is lack of knowledge and procedural skills that exist with the use of new operating room medical technology (Jaffe et al., 2017; Romeo, 2016).
On-the-job training can take many forms for operating room staff, including team-based training, online modules, and virtual simulation, among others. Few studies on the need for training and education in a changing industry exist (Alfredson & Isaksson, 2014). The problem this study serves to address is the lack of earlier scholarship about the most effective strategies, methods, and tools for training and education for surgeon and staff competency with new surgical technologies. Such research could inform practice that could ultimately improve the quality outcome of care, and provider and patient satisfaction.
The gap in the literature is a lack of research about surgeon training with respect to new and sophisticated surgical technologies. Specifically, there is a lack of research on training approaches to meet the needs of operating room staff facing these technologies’ steeper or more significant learning curves. The purpose of the qualitative descriptive study is to understand the experience of surgical personnel in ambulatory surgical centers in northeastern United States who learn new, advanced medical-surgical technology through in-services.
In this literature review, the researcher will provide an extended background to the research problem. The focus of the first section is on the benefits of training programs in both traditional surgical education and robotically assisted surgical education. The focus of the second section is on the lack of general knowledge about effective surgical training methods. The third part involves literature on learning curves in surgical training. The fourth part continues the literature on the benefits of technology in surgical training. The fifth part looks at how factors internal to trainees have been shown to affect surgeons’ training, and how these findings complicate research on the role of technology in surgeons’ training. The literature surveyed indicated a lack of research on precise training methods that are the most effective facing the steeper learning curves of new and sophisticated surgical technology.
Documentation
In order to compile this literature review, a selection of databases was used. These databases and search engines include Google Scholar, PubMed Central, Europe PMC, OVID, and ERIC. The journals used for the literature search included multiple scholarly medical, technological, and combined ones. Some of the journals used are Journal of the American Medical Association, International Journal of Medical Informatics, Journal of the American College of Surgeons, Journal of Surgical Education, Annals of Surgery, World Journal of Surgery, and others. Several key search terms, as well as a combination of search terms, which were input into these databases, included surgical surgery, health care and new surgical technology, training, competence of surgeons, learning curve of surgeons, robot for surgery, and surgeon efficiency. The key terms were used to yield studies that were relevant to the problem and research questions. This review included 115 sources and 89% of the sources were published between 2014 and 2017 to ensure that the latest findings and reports were included, reflecting the most up-to-date information. Older articles were used in the theoretical framework of the study to reflect the seminal studies on adult learning curves.
Historical Content
Recent changes in health care policy and technology have demanded renewed approaches in curricula to medical training and competency assessment (Thomas, Kern, Hughes, & Chen, 2015). However, the older research findings that have been obtained at the time of the rise of technology in medicine allow for identifying the foundations of research in this field. Moreover, the ability to interpret the historical content significantly contributes to the validity of the current research interpretations wince it provides a developmental perspective as per the directions in which the research field is advancing. Therefore, this section primarily addresses studies and articles that were published between 1980-s and 2014 to provide the historical background to the investigated topic
Facilitation of Operating Room Performance
The issue of continuous improvement of medical workers’ performance level has been a central topic in health care research. Some of the studies published in the late 1990-s referred to the necessity of identifying the factors that diminish doctors’ effective work at their practice setting (Tomlin et al., 1999). One of the most influential determinants that lower the level of effective health care was the lack of skills in the hospital personnel. Such means as lectures, observations, and practical training have been identified to significantly expand the scope of skills of both young and experienced health care providers in various settings (McLaughlin, 2012; Patel et al., 2012). This finding implies that the high effectiveness potential of continuous learning, talent development, and training have valuable impact on the performance outcomes and positive patient experience. Such implications apply to the validity of technological use training as an integrative part of operating room performance facilitation in the contemporary health care setting.
Another important element in operating performance facilitation is the issue of patient safety. Since human factor constitutes an influential threat for patient wellbeing and safety when in a surgical setting, the need for increasing reliability of operating room practices was brought to discussion by many researchers. In particular, the expansion of non-technical skills by educational means was found to be an integrative part of increasing proficiency and guaranteed patient safety (Gordon et al., 2012). Similarly, the methods of overcoming the safety threats induced by such human factors as understaffing-related workload, environment, organizational variables, and technology availability were sought (El Bardissi & Sundt, 2012). In addition, the overall working conditions in operating room were addressed by researchers to identify possible ways of improving the efficiency and safety of the provided health care (Matern & Koneczny, 2007). As it is evident now, technological advancement is one of such improving methods.
However, despite such a broad scope of research directions allowing to investigate the opportunities for improved surgeons’ and all operating room teams’ quality of performance, specific ways of achieving this goal were successfully identified. Indeed, more recent publications among the historical content, such as Sadideen et al. (2013), Sanchez-Peralta et al. (2013), and Smyth et al. (2013), are more inclined to investigate the practical aspects of education and training in the domains of technology application to surgical procedures. Thus the inclination toward education and continuous training is addressed as a valuable aspect of high-quality technology-informed health care.
The Integration of Technology into Operating Rooms
Relatively early literature available on the topic of technological integration into the work of the surgical team in an operating room is primarily directed at general articulation of the opportunities provided by technologies in general, and informational technologies in particular. The concept of overall acceptance of informational technologies in work fields was measured in Davis’s (1989) work by identifying the frequency and ease of technology use’s influence on the usefulness of the technological means. Similar aspects were investigated by Venkatesh (2000); motivational, emotional, and controlling characteristics of acquiring technology-using skills were tested for interdependence with usefulness. The study allowed for identifying the importance of practice in using technologies for improved future outcomes. These findings allow for laying the solid background for the necessity of making the use of technology approachable and efficient for users to apply it for performance improvement. The detected significance of practice and training in using technology provides implications for future studies in the methodologies of surgeons’ training for technology expertise.
The integration of robot-assisted surgery to the practice of surgeon was also broadly addressed by the earlier literature as a vital asset for the future development of technologically supported surgical work. As found by Chang et al. (2003) and Okamura (2009), the utilization of robotic surgical tools allows for obtaining less pain and harm to patients and greater accuracy of interventions. However, the lack of performance excellence due to the improper usage skills of surgeons diminished the promising usefulness of technologies. At the same time, other barriers that obstruct omnipresent and effective use of technologies in the operating room is perceived complexity of use and perceived behavioral control (Benmessaoud et al., 2011). Thus, the historical content implies the urgent need for training of the surgical teams to improve their technology usage skills, the level of their ease of use, and the enhanced opportunities for behavioral control.
Surgical Team Training
On the policy side, during the first decade of the 21st century, residency work-hour limits and the rise of competency-based assessment have transformed the way surgeons are trained (Lillemoe, Klingensmith, Darzi, & Taylor, 2017). Heightened awareness to patient safety has also brought added attention to the ways that surgeons are trained (Harrysson, Hull et al., 2014).
Doctors and surgeons are now assessed using a stricter admissions process to select the best-qualified applicants to be responsible for patient care (Association of American Medical Colleges [AAMC], n.d.). This transformation to a stricter assessment process is aimed at preparing medical professionals that understand the dynamic nature of the health care industry and how to positively respond to its fluidity (AAMC, n.d.). The focus of the health care industry on bolstering nationwide surgical training methods has specifically progressed over the first two decades of the 21st century (Cullinan et al., 2018).
During the period between 2000 and 2020, many residents studying surgery had decided to further their studies by partaking in subspecialty training following their residency period for general surgery (Cullinan et al., 2018). Despite the ongoing trend, some directors of fellowship programs, according to Cullinan et al. (2018) have vocalized feelings of their students being unprepared for the fellowship experience. Surgical education in general has been undergoing a transition to this kind of competency-based evaluation and promotion, little data remains on the efficacy of these changes (Clifton & Wulkan, 2015).
Surgical professionals must be trained to adapt to the ever-changing nature of the health care industry (Cullinan et al., 2018). Those changes include the maintenance and care of disease, the move toward minimally invasive surgery and nonsurgical procedures, and a cap on work hours. Pertaining to the latter, the Accreditation Council for Graduate Medical Education enforced the 80-hour workweek in 2003, also requiring a minimum of four days off per month for house officers (Healy, Maxfield, Solomon, Longo, & Yoo, 2018).
These sweeping changes included the hours in which interns were permitted to work, which were not to exceed 16-hour shifts, while postgraduate residents’ hours were reduced from 30 to 28 hours per week (Healy et al., 2018). Although this measure was intended to improve the safety of patients and surgeons alike, it placed a cap on the learning that could be provided within a timeframe.
Current Content
The Learning Process
The transformation to a stricter assessment process begins with academia at its foundation. After undergoing a choosy process of admissions, aspiring doctors and surgeons must apply to medical school. Medical school is then divided into three stages: undergraduate education, residency training, and ongoing education. In addition to students’ academic capabilities, medical schools are now taking into consideration personal characteristics in their selection process (AAMC, n.d.). This includes evaluating whether applicants work efficiently in small groups, their interpersonal communication with others, and their capability to adapt to unique circumstances (AAMC, n.d.).
Specifically, the Medical Admission Test includes two new sections that measure thinking processes and behavioral sciences and social sciences (AAMC, n.d.). If a student is accepted into medical school, he must complete 4 years of undergraduate medical academia, which culminate with a medical degree (AAMC, n.d.). The medical school experience is constantly adapting to reflect ongoing advancements in science, medicine, and technology, along with breakthroughs and social challenges.
Such advancements are particularly necessary for the surgical setting given the acute importance of a high level of expertise and accuracy in such an invasive field. As Rashid (2017) states, new approaches to training in a hospital setting are required to ensure efficacy and safety of educational interventions on site. Indeed, the adult education principles and strategies, as well as well-structured practical surgical training must be intertwined to introduce new frameworks for training. According to the AAMC (n.d.), the health care industry has, as of late, shifted from chiefly focusing on the treatment of acute illnesses to managing, maintaining, and treating chronic conditions, particularly those related to aging. Following the completion of 4-year undergraduate medical school, students must complete residency training if they chose to pursue licensure and/or board certification in a particular area of medicine. These programs may last from 3 to 7 years, but specialty-training can last up to 11 years after a student has received his doctoral degree (AAMC, n.d.).
Education forms the foundation of a surgical resident’s experience, but throughout the educational process, technology may continue to progress. Residents and professionals alike are then tasked with remaining up to date with innovative health care technologies because advancements in surgical technologies have been shown to have beneficial effects (Alfredson & Isaksson, 2014). These advancements can provide medical professionals with information about everything that surrounds the treatment process, from start to finish, occurring internally and externally of the patient (Maier-Hein et al., 2016).
Specifically, the striking growth in the use of medical robots since the mid-1980s has resulted in a wide range of surgical procedures (Jeppson et al., 2015; Taylor et al., 2016). Surgeons perform more quickly and accurately (with fewer errors) on robotic systems. Robotically assisted surgery can be performed more proficiently at a lower workload and with the investment of less mental effort, allowing surgeons greater cognitive resources for dealing with other demands in the operating room (Moore et al., 2015). Surgery requiring related technologies is referred to as smart surgery, which entails robotic surgery and computer-assisted surgery (Morgan, 2014). To be recognized as “smart,” these technologies must offer a level of health or financial benefits that are not solely based in technological innovation (Morgan, 2014). The challenge is that residents and professionals alike must be constantly adapting to and learning how to utilize these technologies.
Operating Room Shortcomings
Despite these demonstrated benefits of advanced surgical technologies, operating room medical technology frequently does not meet the needs of health care providers and patients (WHO 2010). Such technology has become insufficient to address solely the requirements of patients and doctors, as financial restrictions deem implausible for some institutions, particularly those with poor financial status, to obtain specific medical devices (Egeland, Rapp, & Davis, 2017). Simply because a surgical device may offer some level of benefit does not indicate that it can be utilized (Egeland et al., 2017).
A need exists for new educational approaches that address training operating room staff on advanced surgical technology to ensure that health care providers are able to maximize the benefits of these devices when applicable, which could lead to overall improved provider and patient satisfaction (Stanford, Lee, Masaquel, & Lee, 2015). Old models of teaching surgical skills are inadequate to effectively train surgeons to be competent with rapidly progressing technology, which requires the advancement of skills beyond a fixed point in time, such as residency education (Romeo, 2016). This is not a new feat, as the nationwide health care industry has been perceived as being a source of disagreement and dispute, an industry that is outdated considering the needs of the nation, and a combination of both (Grover, Orlowski, & Erikson, 2016). According to Grover et al. (2016), it has been suggested that medical professionals are inadequately trained for their positions. Some universities have been pegged for placing too heavy an emphasis on the academic aspect of the residency training, with students learning more in the academic setting than in a direct environment (Grover et al., 2016). This does not sufficiently provide students with an accurate assessment of the real-life scenario (Grover et al., 2016).
Competency-Based Education
Any universities have strived to combat the aforementioned dilemma by mandating a structure that facilitates the growth of knowledge, attitude, and procedures regarding problem-solving scenarios (Cervantes-Sanchez, Chavez-Vizcarra, Barragan-Avila, Acosta, & Herrera-Mendoza, 2015). Otherwise known as competency-based education, the objective of this learning style is to prepare students for both challenging and unexpected circumstances, as the health care industry is ever-changing (Cervantes-Sanchez et al., 2015; Courteau et al., 2015). Competencies are also used to assess the individual characteristics of health care professionals to determine whether they maintain desirable traits for their positions (Courteau et al., 2015). For example, quality orthopedic surgeons are characterized as being “trustworthy, hard-working and efficient, self-directed learners, detail-oriented, and personable” (Nemani, Park, & Nawabi, 2014, p. 164).
This situation is particularly challenging, as these traits are more likely to be learned during a professional’s childhood and adolescence rather than in academic and clinical-based settings (Nemani et al., 2014). Professionals who maintain these qualities, Nemani et al. (2014) continued, are more likely to succeed in clinical settings, with efficiency assessments including quality evaluations by faculty and peer-reviewed scholarship. Courteau et al. (2015) also suggested that competency-based education includes the assessment of Entrustable Professional Activities (EPAs). These EPAs are jobs or accountabilities delegated to be performed by a student, while unsupervised, following the successful demonstration of the necessary aptitude to do so. This assessment presents an additional layer to the evaluation process.
While competencies measure preferable characteristics of health care professionals, EPAs reference the description of the professionals’ performance, which often demands training that requires the professional to complete the task multiple times prior to proficiency (Courteau et al., 2015; Williams et al., 2017). This learning style can be understood as being aligned with the old saying, “Practice makes perfect.” Although this would be an ideal assessment tool, surgeons perform too many procedures to assume that in every procedure ever performed, aptitude is measured (Courteau et al., 2015). According to Williams et al. (2017), a lack of scholarship still surrounds the process of how supervising surgeons determine whether a resident is ready to perform procedures autonomously with success.
A need also exists for revised and renewed measures of competency to ensure patient safety as technology continues to progress. Patient safety has remained a core concern in the health care industry following a 1999 report issued by the Institute of Medicine titled, “To Err is Human: Building a Safer Health System,” which stated that medical errors resulted in approximately one million injuries nationwide and 98,000 wrongful deaths (Ulrich & Kear, 2014). Despite technological and health care innovations, approximately 400,000 patients annually are thought to die as a result of unnecessary complications associated with medical treatments, coupled with four to eight million instances of serious harm (Ulrich & Kear, 2014).
When these numbers are observed in a day-to-day perspective, approximately 1,096 deaths occur each day, followed by 10,959 to 20,918 bouts of serious harm (Ulrich & Kear, 2014). According to Ulrich and Kear (2014), this number of deaths on a daily basis is comparable to three 747 airplane crashes taking place every day. These high numbers undoubtedly task the health care industry with the need to uncover ways to improve procedural proficiency to ensure safety and success.
Because of these grave challenges, such as the aforementioned deficiency in surgical procedures, different methods of measuring competency have been proposed. Roberts et al. (2006) have elaborated on six core competencies by which all physicians should be measured. These core competencies include patient care, medical knowledge, practice-based learning and improvement, interpersonal and communication skills, professionalism, and systems-based practice (Roberts et al., 2006).
More recently, Moriates et al. (2015) argued that a range of foundational competencies—from basic knowledge of health policy to systems-level design—need to be defined related to health care value that spans all professions and stages of training. Sears et al. (2014) referred to the objective structured clinical examination (OSCE), which offers a means of determining the abilities of a learner. An OSCE entails a particular situation purposely created by the evaluators that enables the learner to demonstrate both knowledge and skills in that situation (Sears et al., 2014). The evaluator dictates both the environment and the situation and assesses the learner according to that learner’s knowledge base. Also included in the assessment are the learner’s perspectives, mannerisms, and behaviors (Sears et al., 2014) to determine whether the learner’s level of people skills complements or counteracts the situation at hand
Effective Surgical Training Methods
Surgical training and education programs have proven beneficial for non-robotic and robotic surgical training alike. Yet a general lack of knowledge about the learning methods that affect the acquisition of surgical skills can lead to devastating effects. With respect to the steeper learning curves posed by advanced surgical technology, research has shown that surgeons themselves have a lack of self-awareness about how they learn (Jaffe et al., 2017). Practicing surgeons use a variety of training methods when learning new procedures and technologies, but there is a disconnect between commonly used training methods and those deemed most effective (Jaffe et al., 2017). This disconnect is further enhanced by the transition from traditional surgical procedures to robotically assisted procedures (Spruit, Band, & Hamming, 2014).
Traditionally, surgical training has entailed an apprenticeship relationship between the resident and the supervising surgeon, which essentially takes place in the operating room (Zendajas, Brydges, Hamstra, & Cook, 2013). According to Zendajas et al. (2013), this relationship is disconcerting because mentoring can be time-consuming and cause harm to the patient because of the resident’s lack of awareness. This situation is particularly prevalent with regard to laparoscopic surgery, which, according to Zendajas et al., requires precise skills that involve exceptional focus.
According to Saidideen, Alvand, Sadideen, and Kneebone (2013), experts in laparoscopic surgery are sufficient at overseeing and assessing their own procedures with a tailored aptitude to identify problems or mistakes. On the contrary, residents do not yet have this ability and tend to look to others–especially their supervisors–to identify their own mistakes and provide solutions (Saidideen et al., 2013). Questions surround the ability to design curricula that integrate effective learning processes applicable to both procedural methods (Spruit et al., 2014). Surgical training has received a lack of theoretical pedagogical attention. Rashid (2017) argued that surgeon-oriented training programs should integrate more educational concepts such as theories of adult learning.
Learning Curves
In the context of this study, a learning curve is understood as the gradual development in surgical performance (Papachristofi, Jenkins, & Sharples, 2016). Learning curves were thought to begin with a hasty increase in the beginning that slows over time as the surgical resident acquires more knowledge (Papachristofi et al., 2016). Academic curiosity surrounding learning curves in surgical training benefitted from the growing interest in the topic, indicating continued assessment of learning curves was needed (Harrysson, Cook et al., 2014). Some aspects of learning curves have received very little attention (Cook, Ramsay, & Fayers, 2004), such as the statistical assessment of learning curves in trials.
Myriad factors are involved in the learning curve, including the learning process of individual surgeons, who all consume and process information at different rates (Papachristofi et al., 2016). The learning curves referenced for various surgeries and procedures are also incompetent because this information is based on unreliable information (Papachristofi et al., 2016). No single procedure has been identified as sufficiently discussing the culmination of the learning process, as justification was based solely on the perspectives of experts or basic investigative materials (Papachristofi et al., 2016). Within the scope of surgery, a learning curve for prospective doctors exists (Khan et al., 2014). This learning curve is recognized as a constant, because both students and professionals are constantly being introduced to new skills pertaining to both knowledge and safety measures (Khan et al., 2014).
According to Khan et al. (2014), the availability of more information about the learning curve may result in surgical training and performance. Measurement of the learning curve consists of two chief factors, which are measurements of the surgery itself and patient outcomes (Khan et al., 2014). The surgery includes factors, including time of completion, success rate, and conversion rate (Khan et al., 2014). Patient outcomes measurements include the duration of the hospital stay, complications during surgery or after surgery, and the amount of blood loss or mortality of the patient (Khan et al., 2014).
One hindrance to researching learning curves in surgical training has been the lack of a standardized definition of learning curves and a lack of standardized methodologies for researching learning curves. Although earlier scholarship frequently references learning curves, what the term entails is not standardized (Subramonian & Muir, 2004). The term was first introduced into the health care industry in the 1980s, following the innovation of minimally invasive surgery (Subramonian & Muir, 2004). Standardization of factors present in a surgical procedure is required. The learning curve relies on the unique abilities of individual surgeons, coupled with their insight about surgical anatomy (Subramonian & Muir, 2004). The degree of the learning curve varies with each procedure and surgery, as well as how often a set of procedures is conducted within a specific timeframe (Subramonian & Muir, 2004). For instance, the learning curve is longer for minimally invasive operations than for open surgery. The ability to identify a standard definition of a learning curve would enable professionals to develop cost-effective means of assessment (Manuel-Palazuelos et al., 2016). This process is certainly a challenge, especially when no optimal assessment of learning is available (Subramonian & Muir, 2004).
In general, data on learning curves is inconsistent, multifaceted, and often ill defined, as the quantification to attain proficiency is variable (Barrie et al., 2014). The number of colonoscopies, for example, required to teach competency is not well established (Ward et al., 2014). Old research argued that 100 to 180 procedures over two to three years are required for competency in colonoscopy (Tassios et al., 1999), while more recent research demonstrates that trainees need to perform 150 to 280 colonoscopies to attain competency (Ekkelenkamp et al., 2016). These data would suggest that learning curves for certain surgical procedures might be increasing. In order for surgeons’ learning curve to adapt properly, then surgeons would have to be honest with their individual performance (Vickers, 2013). This would require some surgeons to admit that they were performing at lower-than-average rates (Vickers, 2013), which may certainly be damaging to any surgeon’s reputation.
In addition to this lack of general research, a specific lack of research on how to approach learning curves when training surgeons on robotic-assisted procedures is apparent. While some have found that robotic procedures can be completed safely by novices with a minimal learning curve (Angus, Sahi, & McIntosh, 2014), limited data are available on that account. Regarding how surgeons gain competency and the way institutional leaders develop programs for robotic-assisted surgical procedures, developing the number of cases performed to achieve competence has yet to be determined, indicating the way learning curves are determined in these situations (Guend et al., 2017; Yamaguchi et al., 2015).
So far, retrospective analyses have been used to address this shortcoming. For example, retrospective analyses showed that in the hands of surgeons with advanced laparoscopic skills, the learning curve to stabilize operation times using robotic systems in surgical procedures in women requiring benign gynecologic interventions is 50 cases (Lenihan, Kovanda, & Seshadri-Kreaden, 2008). The learning curve for robotic pancreaticoduodenectomy (RPD) is 80 cases (Boone et al., 2015). In some instances, a substantial gap occurs in the learning curve.
According to Arora et al. (2014), the learning curve for the following procedures presents a wide range of cases. Between 15 and 100 cases are required for coronary artery bypass surgery; between seven and 35 cases for endoscopic vessel harvesting; between 20 and 135 cases for valvular surgery; and between 100 and 500 cases for vascular neurosurgical procedures. For less complex procedures, fewer cases are required: between five and 40 cases for endovascular vessel repairs; between 15 and 35 cases for video-assisted thoracoscopic surgery; and between 25 and 60 cases for ablation procedures. The immense gap that exists between these numbers is based on the expertise of the surgeon (Arora et al., 2014), which, again, has not been standardized.
Technology in Surgical Training
Much of the recent literature on the use of technology in surgeon training has focused on the potential benefits of integrating new and advanced technology into training programs. Advancements in technology and restriction of surgical work hours have made the use of simulations, virtual reality, robotics, telemedicine, and gaming much more common in surgical training (Evans & Schenarts, 2016). Such advancements have also shifted the learning of basic surgical techniques to the laboratory, freeing up time in the operating room for the acquisition of complex surgical skills. Simulation technology is the most frequently discussed technology, and it has been shown to have benefits for both robotic-assisted and non-robotic surgical training. Other technologies, such as telecollaboration and video game technologies, have also been shown to be beneficial.
Sanchez-Peralta, Sanchez-Fernandez, Pagador, and Sanchez-Margallo (2013) addressed a need to explore the multivariate options surrounding minimally invasive surgery. Minimally invasive surgical methods and the development of technology in health care have become somewhat intermixed, as the two factors often proceed hand-in-hand (Sanchez-Peralta et al., 2013). While a standardized method of surgical training does not yet exist, surgical training that integrates technology is becoming one of the more sought-after methods of learning (Sanchez-Peralta et al., 2013). In the year 2012, the use of technology by health care professionals had increased by 81% (Waltzman, Tadisina, & Zins, 2014).
In addition to the aforementioned technologies, the presence of e-learning, which links surgical residents to Internet resources and needed materials, is becoming more widespread, as residents can connect virtually, no matter their location (Sanchez-Peralta et al., 2013). According to Sanchez-Peralta et al. (2013), the presence of traditional surgical training, coupled with e-learning, may provide an experience that improves the surgical training process. Consequently, surgeons and the health care industry alike are always seeking innovative technologies that may improve the dynamic of the operating room (Khor et al., 2016).
Benefits of Simulation on Surgeon Training
Simulation technology has been shown to have benefits for robotic-assisted and non-robotic surgical training programs alike. This means of learning came about from a rising need for surgical training measures that extended beyond the operating room (Badash, Burtt, Solorzano, & Carey, 2016). This form of training resulted, in part, from new restrictions placed on the number of hours that residents could work per week, coupled with high operating costs (Badesh et al., 2016). As a result, surgical residents needed to learn procedures more efficiently in a shorter time span.
A simulator is a tool used in surgical training processes that reproduce situations in a virtual setting that prospective surgeons will likely encounter in their vocational experience (Badesh et al., 2016). Skills acquired in simulations have significant translational potential because they have repeatedly and consistently been able to transfer to the operating room. Proficiency-based training maximizes this benefit (Stefanidis et al., 2015). Simulation-based mastery learning in medical education can produce downstream results (McGaghie, Issenberg, Barsuk, & Wayne, 2014). Simulation has become a major form of training for proficient use of advanced surgical technologies.
Students can benefit considerably from exposure to surgical simulators designed to train laparoscopic motor skills necessary for successful outcomes (Nemani et al., 2018). Defined, simulation refers to the replication of the procedure of a real method or technique conducted over a period of time (Pedowitz, 2017). Substantial advantages have been witnessed in surgical residents who underwent training utilizing virtual reality simulators (Gaitanidis, Simopoulos, & Pitiakoudis, 2018). Various virtual reality simulators can be utilized, including box trainers, low-to-high fidelity systems, virtual reality systems, and systems using models of live animals (Gaitanidis et al., 2018). Prior scholarship proved that students undergoing virtual reality training benefit more than students who have not received any training (Gaitanidis et al., 2018; Zendajas et al., 2013).
Examples of virtual reality systems include the AccuVein, which is a tool that provides an map of the human vascular system via the skin’s surface, as well as Google Glass, which is a display tool worn on the head similar to sunglasses, that provides a visual of objects superimposed into real-life images (Khor et al., 2016). Virtual reality programs can provide an array of benefits, beginning with the acquisition of skills that are transferable to skills required in the operating room setting (da Cruz et al., 2016; Gaitanidis et al., 2018; Pedowitz, 2017; Vavra et al., 2017). Virtual reality also enables supervisors to observe the performance of surgical residents over time, while recording and tracking their personal metrics (Gaitanidis et al., 2018).
These programs can be adjusted to reflect varying degrees of difficulty and can also be accessed at any time, unlike procedures that are performed in physical operating room settings (Gaitanidis et al., 2018). The feedback provided from these systems may range extensively, including smell, taste, sound, and touch (Khor et al., 2016). Downfalls to these systems exist because they are often available at high costs and oftentimes lack the precision in terms of organ measurements compared with the human body (Gaitanidis et al., 2018). The understanding of the benefits that virtual reality systems can offer the health care industry are not entirely known (Vavra et al., 2017). Training is all forms entail both positive and negative aspects including time, cost, and prioritization of outcomes of each form of training.
Simulation-based training for robotic-assisted surgery offers a range of benefits to trainees, including the acquirement of skills needed to attain surgical competency, improved accuracy, and alternatives to older training methods. Simulation training provides surgical residents with the means of practicing a surgical procedure repeatedly until they achieve precision (Badesh et al., 2016; Rehman et al., 2013). According to Bahler and Sundaram (2014), simulation should be an integral part of robotics surgical training. Simulation allows residents to repeatedly perform these surgical tasks in a virtual space where mistakes do not merit human harm (Badesh et al., 2016; Rehman et al., 2013).
Robotically assisted surgical simulation training has been shown to help for both the acquisition of required skills and the assessment of competency, leading to a much-needed standardization of competency metrics (Arunachalam & Ansell, 2017). Trainees on robotic simulations showed improved accuracy over trainees using traditional non-robotic laparoscopic simulations (Livinti et al., 2015). Training on a virtual reality simulation may also be an alternative to live animal training for future robotic surgeons (Whitehurst et al., 2015).
Simulation has been shown to have training benefits for more traditional, non-robotic surgical procedures as well. Non-robotically assisted procedures require high-level surgical skills and efficient surgical training methods such as simulators that make use of spatial cognitive learning, are required (Jang et al., 2017). Simulators and scope imagers can help build competency and skills acquired by simulation-based training are transferable to the operative setting for a variety of surgical procedures such as laparoscopic cholecystectomy and endoscopy (Dawe et al., 2014; Dubé & Rostom, 2016). These tools are highly realistic, placing residents in a scenario akin to a real-life setting (Agha & Fowler, 2015). Even among students with no prior surgical training, simulators have been shown to help significantly with the acquisition of basic laparoscopic skills (Cavalini et al., 2014). Residents can experiment with the virtual environment to learn how to conduct specialized procedures, along with revisiting certain procedures that are rare or high-risk (Agha & Fowler, 2015).
Researchers Agha and Fowler (2015) used the example of U.S. Airways Flight 1549, a passenger plane that landed in New York’s Hudson River in 2009. The successful, yet challenging, landing of the plane was made possible through simulation, which required pilots to do water-landing drills in a flight simulator (Agha & Fowler, 2015). When compared to surgical procedures, these simulators enable surgical residents as well as professional surgeons to practice procedures in order to ensure success, no matter how tasking the procedures may be (Agha & Fowler, 2015).
Improving simulation-based training for both robotically assisted and non-robotic procedures is always possible. Integrating haptics into medical simulators, for example, would provide surgeons with the important feeling of touch that is missing from most simulators and allow for its integration into telediagnosis or telesurgery systems (Basdogan et al., 2004). Creating more natural interaction of this kind is a crucial part of improving simulations.
Although simulation can provide a quality, cost-effective, safe learning experience for residents and professionals alike, haptic measures are needed to strengthen the realistic nature of the procedure. Integration of augmented reality platforms can improve surgical simulations in this way, as they allow for more of these sorts of interactions with objects (Juanes, Gómez, Peguero, & Ruisoto, 2016). Virtual reality technologies have a range of benefits for simulations. For example, virtual reality used with head-mount displays to create highly immersive simulators enables a completely new generation of surgical training with little motion sickness (Huber et al., 2017). Including the element of touch within the simulation enables the surgeon to achieve a clearer sense of skill proficiency.
Benefits of other technologies
Several other recent technologies have been shown to have positive effects on surgeon training. Maertens et al. (2016) found that the integration of e-learning platforms into surgical training showed either greater or similar effectiveness compared with no intervention and non-e-learning interventions, leading the authors to conclude that e-learning is at least as effective as other methods of teaching surgical skills. Various forms of e-learning include virtual reality scenarios complete with virtual patients, online modules, and a series of resources (Bamford & Coulston, 2016). Possibly the most convenient aspect of e-learning is its accessibility, which is not restricted to a particular time or place (Bamford & Coulston, 2016).
Wearable technology, like Google Glass, has great potential of reshaping health care provision and medical education, in general, and holds much promise in the field of surgery (Ponce et al., 2014; Sultan, 2015). Eye-tracking technology (Merali, Veeramootoo, & Singh, 2017), machine-learning modeling (Fard et al., 2016), video game technology like the Nintendo WiiMote (Ramirez et al., 2017), and 3D printing (Jones, Sung, Weinberg, Korelitz, & Andrews, 2016) have all been tested in training environments with positive results. In robotic skills training, specifically, the use of a recording and replay system is beneficial and more efficient than conventional training methods (Yang et al., 2017). Video-based peer feedback through social networking also appears to be an effective paradigm for surgical education and accelerates the robotic surgical learning curve during simulation (Carter et al., 2015). One of the more researched technologies is telecollaboration.
Telemedicine is the use of technology to transfer data related to health care and medicine virtually from one location to another (Valente et al., 2015). It allows remote surgeons and mentors to facilitate procedures that would otherwise not be attempted due to complexity, difficulty, and lack of local surgical experience. Augmented reality in telementoring (ART) facilitates the transfer of laparoscopic skills from mentors to novices (Vera, Russo, Mohsin, & Tsuda, 2014). Trainers can also make use of telecollaboration and telemedicine to give assistance to trainees when unexpected operative findings are discovered (Ray et al., 2015). Telecollaboration offers the potential to train across great distances and even across borders. VIPAR technology allows for long-distance training of surgeons by mentors and holds potential for international training as well (Davis, Can, Pindrik, Rocque, & Johnston, 2016).
Educational Benefits of Internal Factors
Technologically enhanced training methods have been shown to have benefits for trainees learning both robotic-assisted and non-robotic procedures. Different technologies aid in the acquisition of skills, which lead to surgeon proficiency, competency, and mitigated learning curves. Factors internal to trainees, such as pre-existing experience and skills, and learning abilities, have been shown to affect meaningfully the acquisition of skills and affect learning curves for training.
Dependent on the procedure, experience can serve as a powerful driver of improvement (Maruthappu et al., 2015). Deutsch et al. (2015) showed that among general surgeons, experience mitigates learning curves when transitioning from conventional laparoscopic cholecystectomy to single-incision laparoscopic cholecystectomy. Groenier, Groenier, Miedema, and Broeders (2015) showed that experience combined with advanced technologies influenced learning curves with respect to laparoscopic skill acquisition. With respect to training on robotic-assisted surgical systems, different levels of experience with either robotic or non-robotic procedures will affect surgeons’ experiences of learning curves (Herrell & Smith, 2005). Pre-existing skills have been shown to transfer to robotically assisted surgical scenarios.
Laparoscopic skills appear to readily transfer to a robotic platform, and difficult tasks are actually enhanced, even in subjects naive to the technology (Panait et al., 2014). Previous experience with laparoscopic radical prostatectomy, for example, has facilitated the learning curves for surgeons learning a robotically assisted version of the procedure (Adili, 2017). Some limits exist to the ways preexisting experiences translate to robotic-assisted training platforms, because the procedures require specific technological knowledge and experienced surgeons who possess domain knowledge. The experienced surgeons need to acquire technical knowledge under supervision (either in simulated or clinical environment) to transition successfully to robotic surgery, whereas novice surgeons need to acquire both domain as well as technical knowledge to become competent in robotic surgery (Sood et al., 2015).
Other factors affecting the success of surgeon training include learning abilities, motivation, and availability of resources. Research has shown that candidates for surgical programs demonstrating abilities conducive to learning are more likely to be admitted in surgical training programs in the first place, affecting their rates of success (Gallagher et al., 2014). Aho et al. (2015) showed mentor-guided self-directed learning stimulated surgical residents to practice with greater frequency, leading to significantly improved, minimally invasive surgical skills without significantly increasing the need for faculty-led instruction. Finally, lack of resources, lack of incentives created by the health care market, lack of communication between faculty and residents, and lack of scrutinizing of surgical technologies’ cost-benefit measures all impact training programs (Champagne, 2013).
Theoretical Framework Literature
Any research must be properly equipped with solid theoretical foundations to ensure consistency of the investigation procedures, choice of design, methods, data collection techniques, and ultimate results analysis and interpretation. The correct choice of theories allows for proper guidance of the overall research in the direction set by the researcher’s purpose. The theory of andragogy introduced by Knowles (2015) is central to the current study. Since the primary goal of this qualitative descriptive study is to investigate the training patterns of professionals involved in the surgical practice at health care facilities, the particularities of adult learning are of significant importance. The theory of andragogy allows for differentiating between the characteristics of educational approaches in children and adults. The various forms of learning available from adult education allow for versatile utilization of training interventions for the most effective outcomes within the realms of knowledge expanding, skills development, and expertise gaining.
However, the multiple benefits of the application of this theory to the field of medicine have been addressed by other researchers. Indeed, such an approach, in the opinion of Waring and Bishop (2015), leads to intensified standardization of skills, as well as strives for obtaining efficacy in surgeon’s work. The efficiency-driven direction of medical staff learning by means of andragogy allows for obtaining better results in the working setting. As claimed by Whitfield (2015), general practitioners and surgeons exposed to the standardized training perform under better control and deliver more standard results.
The theory of andragogy assumes that people in their adulthood possess a particular set of knowledge, skills, and attitudes that are used as the background for designing specific techniques for learning. The assumptions that adult learners have obtained vast experience both life and professional, can act independently and with self-direction and self-control, and motivate their educational behavior by the requirements of the everyday practical use of the obtained knowledge or skills leads the theory (Merriam, 2001; Ozuh, 2016). Derived from these ideas, the learning process for adults should occur through the integration of adults’ interest in problem-solving and immediate application of knowledge to practice, perception of the information in the context and within the observable situations, and internal motivation (Merriam, 2001; Ozuh, 2016). Thus, the utilization of the theory of andragogy allows this study to evaluate the perception of medical staff’s learning experiences against the criteria applicable to adult learning.
Methodology Literature
Meaningful education research begins with compelling questions (Christancho, Goldszmidt, Lingard, & Watling, 2018); in recent years, qualitative research methods have become increasingly prominent in medical education. The study included discussion on the standardized method of surgical training that does not yet exist; surgical training that integrates technology has become one of the more sought-after methods of learning (Sanchez-Peralta et al., 2013). Even though the researcher is in the process of researching other and previous medical education researchers with qualitative methodologies, as testified by Christancho et al. (2018): “Qualitative research examines how things unfold in real world settings.”
Studies involving teaching or training and learning might be conducted using one of three approaches: quantitative, qualitative, and mixed methods. Each method is used to obtain a scholarly understanding of the phenomenon under study (Yin, 2017). Literature reviewed in this section showed that various research methods were involved in the study of education and training of health care workers. Isolating the surgical staff members who work in the operating room serves to focus the education and training on a staff that maintains a stressful schedule while trying to keep up with rapidly advancing technologies.
The field of health care is broad and all encompassing. Focusing solely on the scientific aspects of health care resolves issues of health that depend upon the objective, evaluative nature of health. Yet the nature of positive health care rests upon the empathetic dedication of the health care workers who work in profit-oriented businesses. The focus of this study was on the experiences of health care workers dealing with the impersonal, robotically engineered medical-surgical technologies now dominant in the operating room.
Research Design Literature
This study involved the use of the qualitative method and the descriptive design. The choice of appropriate design within the chosen methodology is crucial for a study since it predetermines the characteristics of data that will be collected and the ways it will be analyzed and interpreted (Groenewald, 2004). As Maxwell (2012) claims, the designs within qualitative methodology are structured as interactive strategies. However, the descriptive design entails observation of the investigated phenomena without intrusion for the purpose of identification of objective data. As Yin (2017) states, each method and design serves a specific purpose; consequently, a descriptive design, as its title implies, serves the purpose of describing the certain phenomenon, situation, or population with the aim of answering the research questions related to the ways something happens and the reasons behind it.
Conclusions
To conclude the literature review conducted in this section, one should emphasize the availability of a wide range of scholarly sources, academic publications, and other literature on the investigated topic. The literature on the technologies and education in the medical setting is relatively new; the historical content was retrieved from the sources dated not earlier than 1980-s, which is conditioned by the recent advancement in the robotic technologies and their application to the surgical work. As the current content review showed, the majority of practice- and training-related sources were published in the late 2010-s. At the same time, the characteristics of the research methods and findings observed in the literature review allow for noting that there is a gap in direct addressing of training opportunities for teamwork in the operating room for better technology use. Thus, the relevance of the current study is enforced by the identified literature gap. As for the methodology, theoretical framework, and design literature, the collected sources constitute a solid ground for the successful conducting of the research by scholarly-supported means.
Chapter Summary
A lack of early scholarship about the training for robotic-assisted surgical procedures and the learning curve needed to develop competency with surgical technology led to concerns regarding patient safety. This literature review included information about earlier scholarship that indicated the known data, while also indicating the gap in the literature. Earlier scholarship about learning curves in using robotic systems took the form of retrospective analysis, which was obtained from this literature review. Current literature about technologically assisted medical training, such as that in virtual environments, is broad. The current literature might be valuable for future research to draw upon literature regarding the acquisition of expertise, mastery learning, and proven theories in all educational and cognitive psychology literature based on the topic in question (McGrath et al., 2018).
This literature review included background into the nature of the research problem through an investigation of relevant areas. The focus is on the experience in training programs in advanced surgical technology as the participants describe them. Next, the literature review included information about the lack of general knowledge about effective surgical training methods. The third part of the review included information about learning curves in surgical training, followed by the benefits of technology use in surgical training. The fifth section included literature that assessed how these findings complicated research concerning the role of technology in surgeon training. Chapter 3 includes a discussion about the methodology of this research, detailing the processes involved in data collection and analysis.
Research Methodology
The phenomenon under study involves understanding the experience of surgical personnel in ambulatory surgical centers in the northeastern United States attending in-services to learn new medical-surgical technology. Chapter 3 includes a thorough description of the qualitative descriptive approach and its appropriateness for studying the topic. The chapter also presents the study population and rationale for selection of the sample, followed with the rationale for the selection of the methodology, a description of procedures for data collection and analysis, and credibility and transferability of the instruments used for the study. A summary concludes the chapter.
Research Method and Design Appropriateness
The purpose of the qualitative descriptive study is to understand the experience of surgical personnel in ambulatory surgical centers in the northeastern United States who learn new, advanced medical-surgical technology through in-services. Under the heading of research methods are three basic types: quantitative, qualitative, and mixed design. Determining which method to use helped in the selection of the design, especially after reading the research questions and the type of search required.
Quantitative Method
The quantitative method was not appropriate for this study. Researchers use a quantitative method to focus in on a specific question or test a hypothesis. For these reasons, quantitative research uses a form of measurement to quantify the responses to the research question(s) to objectify the question under study or ensure greater generalization. Different kinds of questions require a different method. The quantitative researcher needs to organize the research question carefully to ensure clarity of the question so that the results align with the entire study.
Qualitative Method
If a researcher is working with another type of question such as a question involving ideals, attitudes, or perspectives, the qualitative method is more appropriate for dealing with the open-ended nature of the human mind and experience. The questions involved a how or why form of inquiry, requiring both an open approach to potential responses from participants and more interactive questioning on the part of researcher and participant.
The participants do not represent a random selection of individuals but rather a more purposive sample who would have background or experience with the research study in order to ensure helpful responses. Qualitative research may also involve a variety of forms of data: oral or textual data, written examples, dreams, and perceptions—all of which escape standard forms of measurement. The strength of the analysis of such data does not rely upon mathematic or statistical calculation as in quantitative methodology but upon other forms of analysis more suited to the topic to ensure validity.
Mixed Method
The mixed method is useful for researchers with more complex studies, involving both an open approach to human ideas and perspectives as well as specific analysis of aspects of the study. A mixed method requires the researcher to be knowledgeable in both quantitative and qualitative methodologies as well as capable of integrating the results of both forms of results. As a result, the mixed method approach was be used in the study.
Because the nature of the research questions all involves responses dealing with how and are open to a variety of responses emerging from the participants’ experiences and perceptions, the qualitative method is most appropriate for this study. Using the qualitative method involved one of the designs for qualitative research. A few of the more common designs are the phenomenological design, ethnographic design, a grounded study design, and a descriptive design.
Appropriateness of Design
Qualitative research is used to explore meaning and interpret constructs through a holistic perspective (Jeanfreau & Jack, 2010). Use of the qualitative method enables the researcher to interpret the construct, or phenomenon, of focus–training approaches for operating room staff competency of new medical-surgical technologies–through the perspective of a holistic group who experiences the phenomenon–anesthesiologists, CRNAs, and surgical technologists. A qualitative method permits the understanding of complex phenomena from the perspective of the participants’ experiences rather than fixed categories and quantities, characteristic of quantitative methodology (Simon, 2006).
The qualitative design chosen to address the purpose of the study and research questions is a qualitative descriptive design. A descriptive design is an appropriate design when the researcher wishes to conduct a qualitative examination of experience, attitude, or phenomenon. Yin (2017) noted the selection of a qualitative research method was the optimal approach to address a problem statement and collect data to answer the research questions that asked how.
Research Questions
A qualitative descriptive design is most appropriate to address the purpose of the study and research questions. An improvement in the training of advanced equipment would lead to a staff willingness to use, staff use knowledge and skill as they contribute to a protocol, staff knowledge-sharing willingness, staff job satisfaction, patient safety, and patient satisfaction. The research questions of the present study include the following:
- RQ 1: How do surgical personnel describe their experience of learning new, advanced medical-surgical technology through in-services at ambulatory surgical centers in northeastern United States?
- RQ 2: How do surgical personnel at a selected ambulatory surgical centers
- experience in-services as a means to learn to use new, advanced medical-surgical technology ?
- RQ 3: How do surgical personnel describe the effect of learning new, advanced medical-surgical technology through in-services with respect to their self-described confidence in their skill.
Population and Sample
The study involved the population directly responsible for surgical care in accredited ambulatory surgical centers. The population included surgeons, surgical technologists, anesthesiologists, and CRNAs, working in the northeastern part of the United States. Because people working in this profession are over the age of 18, the individuals selected for the sample were of appropriate age. The estimate of the population is validated by the specifications of priorly conducted studies and included 10 participants representing the various roles of the operating team (Arakelian et al., 2011). Thus, the number and age of participants sufficed the requirements of the study and present a reliable sample for credible findings.
Using purposeful sampling, the researcher intentionally selected participants who represented abundant but different perspectives of the phenomenon and fit the purpose of the study (Smith, J. et al., 2009). Small samples are suitable for qualitative studies, according to Smith, J. et al. (2009), because the sample represents an in-depth perspective of the topic. A total of 10 surgeons, anesthesiologists, CRNAs, and surgical technologists comprised the intended sample size.
Inclusion criteria for participation in the study were established: (a) Participants in this study had experience working in the surgical center and (b) attended in-services on new technologies by at least two different modalities. The training occurred (c) within the last two to three years. The researcher attempted to ensure, if possible, that (d) participants had experience with in-person/team-based training as well as technologically mediated training. In that way, (e) the participants could speak meaningfully to the advantages and disadvantages of either an on-the-job or in-service or a technology-based method of learning, using a relevant basis for comparison.
Informed Consent and Confidentiality
Protection of human research subjects was assured for the duration of the study, beginning with the informed consent (see Appendix C) form. As part of the informed consent process, participants who met the inclusion criteria were advised they must agree to the informed consent form posted on the first page of the questionnaire hosted by SurveyMonkey. The recruitment flyer (see Appendix B) included a description of the purpose of the study and an explanation of the study procedures. The flyer also included a declaration that every effort to protect participants’ privacy was made as well as an assurance that no personal risk would accompany participation in the study.
The participants received contact information in the informed consent form, should participants have any questions prior to signing. The informed consent form establishes the participant’s permission for participating in the study. The informed consent form also contained an assurance that participants could withdraw from the study at any time before or during the completion of the questionnaire by simply logging off the SurveyMonkey site.
To begin the study, the researcher recruited participants through social media and using the snowball technique to provide the link to the questionnaire hosted by Survey Monkey. The researcher did not know the identity of any participant because all data were presented anonymously in aggregate from SurveyMonkey. This study was a project conducted with the strictest confidentiality
Instrumentation
The primary source of data collection for this study consisted of textual data compiled from the participants’ responses to a questionnaire. To accommodate the availability and convenience of participants and ensure confidentiality of participants’ responses, the questionnaire afforded opportunities for the participants to elaborate on their responses (Machtmes et al., 2009; Patton, 1987). The questionnaire was derived from material obtained from the literature review and customized according to the research questions.
To obtain descriptions to understand more clearly the phenomena under research, participants responded to open-ended questions (see Appendix D). The aim of the questionnaire was to elicit information from the participants regarding their perceptions of and insights into the effectiveness of education and training interventions currently used for initial training of surgical staff in the use of advanced surgical technologies.
Credibility and Transferability
Trustworthiness
Credibility and trustworthiness in qualitative research studies refer to credibility, dependability, confirmability, and transferability of study procedures and findings (Gay et al., 2006). For qualitative research, the degree to which the results accurately represent the phenomena determines validity (Patton, 2001; Simon, 2006). Validity in qualitative research can also be described as the extent to which a test measures the research goals and objectives (Whittemore, Chase, & Mandle, 2001). By remaining in strict alignment of material and using a third-party vendor to help maintain privacy and confidentiality, a professional relationship with participants could be maintained.
Credibility
Internal validity refers to the extent to which effects of the study represent truth and reality instead of a phenomenon marred by extraneous influence (Vagle, 2009). In qualitative research, the researcher intentionally expressed validity by attending to the participants, the text, and the case or situation studied. The researcher followed systematic procedures for perspectives to be clear (Vagle, 2009). Trustworthiness of the instrument indicated the strength and validity of the findings.
Transferability
Transferability refers to the ability of other researchers to apply the study findings and conclusions to similar research situations (Patton, 2001). The uniqueness of a study may inhibit direct replication in other contexts. Generalization in qualitative research can be limited because no two people are the same (Mertler & Charles, 2006). The use of structured procedures allows for the replication of the study in different yet similar contexts but will not necessarily generate similar responses.
Dependability
The dependability of data depends on the strength of the validity of the study, the questions, and the participant’s responses to the questions (Mertler & Charles, 2006). Participants were asked the same research questions to ensure objectivity and consistency in the study. Participants’ descriptions of their perspectives should yield dependable and credible responses (Guba & Lincoln, 2005). During data analysis, the use of verbatim responses grounded data interpretation in order to answer the research questions in a trustworthy fashion (Groenwald, 2004).
Confirmability
To begin, rigor and trustworthiness enhance the confirmability of a study. Rigor in a research study is necessary because qualitative studies are not subject to the replicability of the quantitative study. As a result of the nature of qualitative studies, other aspects of a study must attest to the quality and trustworthiness of the design. The qualitative researcher must acknowledge “the naturalistic design is emergent” (Lincoln & Guba, 185, p. 317). To test the rigor of a qualitative study, the researcher must develop skills in reinforcing the rigor of the research process. Rigor can be induced from the characteristics of feasibility, integrity, and believability (Ryan, Coughlan, & Cronin, 2007). The three factors of feasibility, integrity, and believability indicate a study is rigorous and trustworthy, affecting sound results.
Data Collection
A qualitative research methodology with a descriptive design was used to investigate current training approaches used in ambulatory surgical centers located in northeastern United States. Raw data reduction took place through identifying data patterns and developing a framework to extract the essence of what the data are revealing (Patton, 2001).
Qualitative data analysis involves an inductive approach (Gay et al., 2006; Patton, 2001). The use of Braun and Clarke’s (2012) six-step process for thematic analysis to analyze interview content allows for induction to occur in order to understand the phenomenon under study. That phenomenon consists of descriptions by participants of training approaches for surgical staff in using advanced surgical technology in order to meet competency requirements. The following procedures were applied to analyzing each transcript:
- Become familiar with the collected data: responses to the questionnaire are read and reread. While reviewing the data, notes are recorded, documenting the researcher’s observations and thoughts.
- Identify codes pertinent to the research questions. Codes or a label are used to explain implicit and explicit meanings for each participant who is the unit of research.
- Categorize excerpts. Excerpts are analyzed and combined to develop themes relevant to the research questions.
- Quality of themes. Once the researcher identifies the themes, they review the codes to determine the quality of themes generated. Themes that contain pertinent and important ideas from the data set and are relevant to the research question are kept; others are eliminated,
- Develop theme definitions. Each theme is defined to reflect concisely the key elements important to the results. Finally,
- Write a narrative about the finalized themes linking themes together to support thick and rich descriptions to answer the research questions.
Themes derived from the descriptions generated provide greater understanding of the experiences of the participants in training competencies for surgical staff. Last, this means the researcher uses each source of data to gain a well-rounded understanding of the data as a whole (Gallivan, 1997). The themes comprise the results of this research.
Chapter Summary
This qualitative descriptive study was intended to explore the experience of training and education for surgeon and staff competency with new surgical technologies. The study involved a sample population of 10 surgeons, anesthesiologists, CRNAs, and surgical technologists. The participants completed a questionnaire to express and explain their experiences of learning skills for working with advanced technology. Different education or training modalities can be used to prepare staff to operate new technologies in actual practice in the operating room. The focus of the study was to derive insights to improve hospital education/training protocol (see Appendix E).
Findings from this study may shed light on the means of enhancing knowledge and skill acquisition regarding the use of modern technology by surgeons and the surgical team as well as on the hazards that may appear (Matern & Koneczny, 2007). According to this strategy, the research might help leaders develop “a strong motivation” among the staff in terms of using new surgical technology (Christensen, 2013, p. 251). The results could also be used to inform policy and purchasing practices in attempts to make rapid improvement in the use of new equipment. The ultimate result would be the application of non-technical skills, the success of surgeries (Gordon et al., 2012), and the satisfaction and safety of all.
Having reviewed the methodology involved in the study, the involvement of others in the research process became clear. I realized the protocol and the questions to which participants responded, would yield insights into the perceptions of the surgical staff to forms of educational delivery. The next chapter contains the results of the analysis. To clarify the results, tables and graphs will be used to convey the significant elements.
Analysis and Results
The collected data analysis and the results of the conducted research are presented in the fourth chapter. The findings obtained in the course of the qualitative descriptive study are presented through research questions introduction, data collection procedure, demographics, and data analysis description. The study involves understanding the experience of surgical personnel in ambulatory surgical centers in northeastern part of the United States who learn new, advanced medical-surgical technology through in-services and on-the-job-training. The findings are presented in tabular and charts.
Research Questions
The research questions of the present study are as follows:
- RQ 1: How do surgical personnel describe their experience of learning new, advanced medical-surgical technology through in-services at ambulatory surgical centers in northeastern United States?
- RQ 2: How do surgical personnel at selected ambulatory surgical centers experience in-services as a means to learn to use new, advanced medical-surgical technology?
- RQ 3: How do surgical personnel describe the effect of learning new, advanced medical-surgical technology through in-services with respect to their self-described confidence in their skill?
Data Collection
The data collection began as soon as the proposal was approved by the University of Phoenix Institutional Research Board. Announcements regarding the study were posted on social media and spread through word-of-mouth. The flyers included descriptions with the purpose and procedures for accessing and completing the questionnaire. As part of the recruitment process, each participant who met the inclusion criteria was able to log into the URL to access the questionnaire hosted by SurveyMonkey.
Each participant acknowledged and affirmed informed consent by checking the appropriate box on the first page of the study website to receive access to the questionnaire. Those who did not provide consent did not receive access. Participants in the study voluntarily continued through the questionnaire to receive the thank you note at the end of the questionnaire. Broad and open-ended questions helped the participants to concentrate on the topic.
Demographic
Participants in this study (a) had experience working in the surgical center and (b) attended in-services on new technologies by at least two different modalities. The training occurred (c) within the last two to three years. The researcher attempted to ensure, if possible, that (d) participants had experience with in-person/team-based training as well as technologically mediated training. In that way, (e) the participants could speak meaningfully to the advantages and disadvantages of either an on-the-job or in-service or a technology-based method of learning, using a relevant basis for comparison. The working experience and the level of expertise in the surgical field, as well as the characteristics of training experience were critical to the study. Such demographic characteristics as age, race, gender, or marital status were not collected since they were of no relevance to the research purpose and intended outcomes. Only profession-related information, such as the position at the facility, the type of organization-based training the participants attended, and their reflection of the experience they obtained during the training were collected during the questionnaire.
Data Analysis
The research data obtained from the participants in the course of conducting the questionnaire was analyzed by studying each questionnaire answers upon completion. The researcher attended to each questionnaire and systematized the answers separating them according to the question number and the similarities in answers. Since the questionnaire contained broad and open-ended questions, the answers to them required thoughtful and determined attention of the researcher. The analysis of the answers on the basis of the characteristics and perceived attitudes of the participants was carried out to identify the core themes in the population’s attitudes. Open-ended question answers were grouped by theme and presented in the form of bar charts to demonstrate and interpret the percentage of each theme in the responses of the participants. The answers to the closed ended questions were presented in the form of pie charts to demonstrate the percentage of particular answers among the entire studied population sample. Such a systematic and thorough approach allowed for laying a solid background with vividly illustrated data for the following step of results representation.
The first question sought to understand respondents’ current role/position by asking them to “describe your role in your current organization and department.” Out of the 13 participants, three were surgeons, two were Surgical Technologist, two were Operating Room Nurses, two were Anesthesiologists, one was Occupational Therapist, one was Certified Registered Nurse Anesthetist (CRNA), and two did not indicate their current positions. Figure 1 below shows participants’ distribution per current role/position.
Results
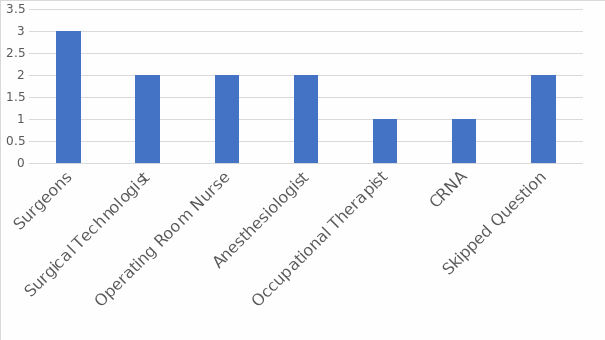
Participants’ Education and Training
To understand participants’ education and training regarding new medical-surgical technologies, they were asked to choose the education and training they had received or continue to receive as a surgeon, anesthesiologist, CRNA, surgical technologist, operating room nurse, or “other.” The choices given to the respondents included In-services, On-the-job-training, or All of the above. Out of the 13 respondents, 2 (15%) did not respond to the question while 10 (77%) indicated that they had used both In-services and On-the-job-training. Lastly, only one (8%) respondent said that s/he had used in-services (see Figure 2 below).
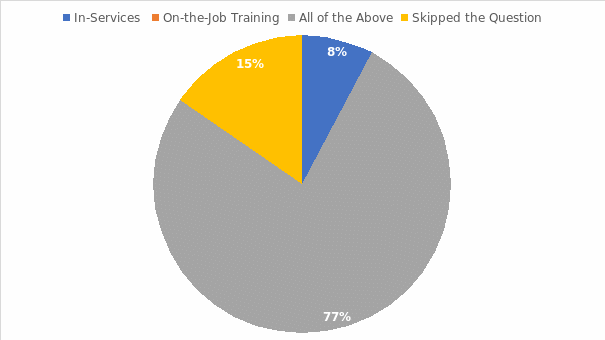
Experience of Learning New, Advanced Medical-Surgical Technology Through In- Services at Ambulatory Surgical Centers in Northeastern United States
Shortcomings and Drawbacks of In-Service Training Strategies
One of the goals of data collection by means of questionnaire was to explore the perceived reasons for drawbacks and imperfections of the training sessions the participants attended. To understand the shortcomings and drawbacks of in-service training strategies, the participants were asked to describe their experience by answering the following question: “From experience, what are the shortcomings and drawbacks of in-service training strategies?” Analysis of their responses led to the emergence of the following themes: inappropriate methodology and curriculum and lack of follow-up and motivation. Thus, a closer explanation of each of these two themes is relevant.
Inappropriate methodology and curriculum
Some of the participants emphasized that the methodology and curriculum utilized in in-service training were inappropriate. For example, Participant 10 complained of the inappropriate curriculum. Participants 1, 7, and 13 noted that in-service training was characterized by “lack of motivation, inappropriate curriculum, inappropriate methods, and lack of follow-up.” Lastly, Respondent 12 complained of “Lack of motivation, Inappropriate methods, and Lack of follow-up.”
Lack of follow-up and motivation
Participants 3, 6, 8, 9, and 11 indicated “lack of follow-up” was a major impendent to in-service training. On the other hand, Participant 5 complained of “lack of motivation.” Overall, majority of the respondents (38%) perceive “lack of follow-up” as the key hindrance to in-service training (see Figure 3). Next, 23% of them described “Lack of motivation, Inappropriate curriculum, Inappropriate methods, and Lack of follow-up” as drawbacks of in-service training. On the other hand, 8% of the participants noted that “lack of motivation” hindered their participation in in-service training. Similarly, 8% of respondents attributed the training to “inappropriate curriculum” while another 8% complained of “Lack of motivation, Inappropriate methods, and Lack of follow-up.” Lastly, 15% of the respondents did not describe the drawbacks associated with in-service training.
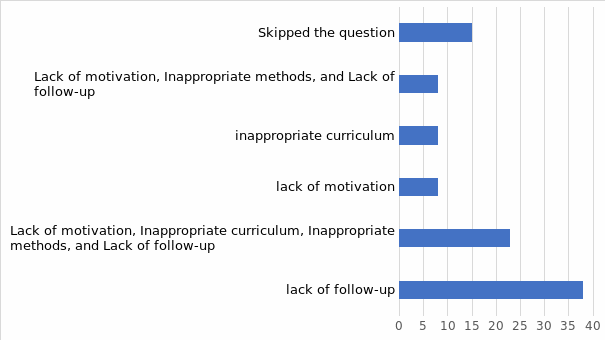
Ways of Addressing Shortcomings and Drawbacks of In-Service Training Strategies
To understand ways of addressing shortcomings and drawbacks of in-service training strategies, participants were asked to describe “How can the shortcomings and drawbacks of in-service training be improved to increase the quality of performance of future/novice operating room staff members?” Analysis of their responses led to the emergence of four themes— manufacturers’ representatives as trainers, follow-ups, the adequacy of trainers, and motivation and interactive instruction.
Manufacturers’ representatives as trainers. The participants suggested various ways of addressing the shortcomings and drawbacks of in-service training strategies. Participant 1 indicated that “training should include appropriate and strict curriculum” while the second respondent skipped the question. The third respondent noted that “there should be scheduled dates for the representative of the manufacturers to come in for follow-ups and possible retraining.” This implies that the respondent perceives the representative of the manufacturers as being the best trainers— possibly because they have experts who are well-versed with how the instruments and the equipment work. The fourth respondent did not provide ways of addressing in-service training challenges.
Follow-ups. The sixth respondent suggested that “follow-up should be encouraged.” Similarly, Participant 8 said that “the manufacturer should always schedule follow up training to ensure the efficiency of the staff in handling the equipment.” Respondent 9 agrees that “by making follow-ups available,” the quality of performance of future/novice operating room staff members could be improved. Participant 11 emphasized that “follow up will help increase competence. The company or manufacturer can schedule follow up after each training as continuing education for a better outcome.” These responses denote respondents’ inadequate skills and knowledge regarding the use of instruments or equipment was attributed to the failure of the trainers to try to understand whether participants understood the curriculum or not. The response further implies that the participants believe that they can master the essential skills if the trainers did a follow-up.
Adequacy of trainers. Participant 7 noted that “The reps from the companies may have difficulty with the dynamics of the operating room. They should be educated on how OR works. Follow up should be scheduled after the training.” This implies that although experts sent by manufacturers to train hospital personnel are well-versed in how the instruments and equipment work in the factory setting, they are not well-versed in using them in the operating room since they are not healthcare professionals. Participant tenth stated that inadequate quality of performance of operating room staff members is because “sometimes the equipment is not discussed in the training session.” This means that part of the training is more focused on the theoretical aspects of the instruments and equipment rather than the practical component.
Motivation and interactive instruction. The fifth participated suggested that in-service training should “create creative, insightful, and interactive in-service training.” This indicates that the previous curriculum provided to the participants was inappropriate and did not motivate them to learn the skills needed to operate the instruments and equipment. Participant 12 noted that the quality of performance of future/novice operating room staff members could be improved if “Before each in-service, the company provided light refreshments and always use a media that will have clear visual and audio.” In agreement, Participant 13 emphasized that “Motivate people by serving some refreshments. Go to the point, talk about the focus instrument or the equipment only. Teach with the right media. and try to follow up to encourage others to participate.” Participants’ responses highlight the importance of motivating trainees to help them stay on track and use of interactive instruction to keep trainees focused.
Shortcomings and Drawbacks of On-The-Job-Training Strategies
The participants further described shortcomings and drawbacks of on-the-job-training strategies. According to Participant 1, the short-comings include “ineffective trainer, team disturbances, rushed training, low productivity.” Participant 2 and 4 skipped the question while the third respondent complained of “team disturbances, rushed training, and low productivity.” The fifth and thirteenth respondent described on-the-job-training as characterized by “Rushed training” while Participant 6, 7, and 11 described the drawbacks as “Team disturbances and Rushed training.” Participant 8 and 9 complained of “Team disturbances.” Participant 10 described on-the-job-training strategies as having “Ineffective trainer.” The twelfth respondent complained of “Ineffective trainer, Team disturbances, Rushed training.”
Overall, majority of the respondents (23%) attributed on-the-job-training strategies to “team disturbances and Rushed training.” Next, 15% linked this methodology to “Rushed training” while a similar percentage (15%) complained of “team disturbances” while 15% did not answer the question. Additionally, 8% of the respondents “ineffective trainer, team disturbances, rushed training, low productivity.” Similarly, 8% of them described the strategy as having “ineffective trainer” and one of them (8%) complained of “team disturbances, rushed training, and low productivity.” Lastly, one respondent (8%) saw on-the-job training as characterized by “ineffective trainer, team disturbances, rushed training.” These results are displayed in Figure 4 below.

Ways of Addressing Shortcomings and Drawbacks of On-The-Job-Training Strategies
To understand ways of addressing shortcomings and drawbacks of in-service training strategies, participants were asked to describe “How the shortcomings and drawbacks of on-the-job-training are improved to increase the quality of performance of future/novice operating room staff members.” From an analysis of their responses, the following themes emerged: timely training by qualified staff and minimizing distractions.
Timely Training by Qualified Staff
Participant 1 stated that “All training should be scheduled ahead of time to accommodate most employees. The team should be given strict rules to adhere to instructions from the trainer.” This means that the respondent felt that majority of the employees were not told in advance that the training was taking place and, thus, a lower turnout. In support, the third respondent emphasized that “The training should be conducted by the most experienced staff member. Enough time should be allocated for the training, and the schedule must be made to accommodate most staff members or all.” Therefore, apart from timely informing employees about upcoming training, the respondent agrees that adequate time should be allocated for effective learning of the skills.
The need for competent trainers was further highlighted by Participant 5, who said that “personal providing on the job training should be well-versed and show complete competence.” This implies that a trainer who is well-versed with knowledge and skills regarding the use of instruments and equipment in the operating rooms can effectively teach the health workers. The seventh respondent further noted that “All staffers must take the training seriously. They should give more time for training” while Participant 8 emphasized on the need for “Strict handling of training time and participants.”
Timely Training by Qualified Staff is a recurrent theme as highlighted by Participant 10 who emphasized that “Experienced person should be the one teaching” and the eleventh respondent who noted that “They should allocate more time and enforce time and location.” Additionally, Participant 12 emphasized that “The on the job training team must deliver the training using a well-experienced employee and give enough time for the training. All employees participating in the training must be cautioned about cell phone use.” Lastly, Participant 13 agreed that “Allowing enough time for training will encourage others.”
Minimizing Distractions
The second theme that arose from the participants’ response is the need to minimize distractions. The sixth respondent noted that “All team members must be discouraged from socializing during training.” In support, Participant 9 stated that “All staff members must take training seriously and not try to socialize during training.” The minimal distraction allows the trainees to be mentally focused on what is being taught.
Participants’ Experience In-Service
To understand whether personnel experience in-service as a means to learn to use new, advanced medical-surgical technology, they were asked to state whether the “in-services training available to the staff members are sufficient to prepare you for your role/s, especially as you often encounter crucial circumstances and manage complicated medical equipment in your daily tasks.” Out of the 13 respondents, 11 (85%) of them agreed that in-service training is essential in learning to use new, advanced medical-surgical technology while 2 (15%) skipped the question (see Figure 4). Similarly, 85% of them agreed that on-the-job-training available to the staff members are effective in helping them learn to use new, advanced medical-surgical technology while 15% did not respond to the question (see Figure 5).
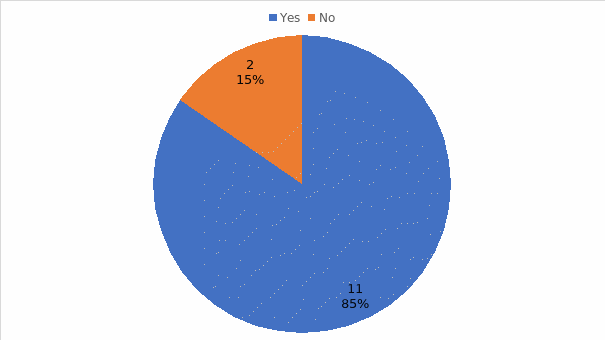
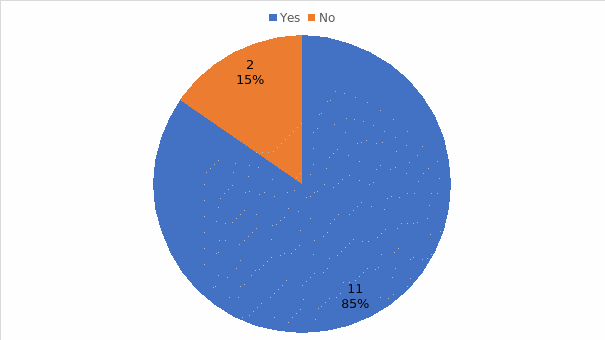
Effect of Learning Advanced Medical-Surgical Technology on Participants’ Confidence
Participants were asked to describe “How do the in-services and on-the-job-training and education strategies help the staff members perform their duties and contribute to staff competence and efficiency inside the operating room.” Research participants shared a range of experiences and beliefs regarding the impact of learning new, advanced medical-surgical technology on their confidence, competence, and efficiency. For example, Participant 1 stated that “It helps shed more lights to how to use the instruments and or equipment. More education, the better experience.” This implies that the first respondent saw the learning experience as being important in improving their skills regarding the use of instruments and equipment. Therefore, the participant felt more confident in the use of the instruments and equipment following the in-service training.
Participant 2 did not respond to the question while Participant 3 described the in-service training as helpful “in refreshing old skills and applying new ones.” Like Participant 1, it can be seen that Participant 3 understands in-services and on-the-job-training as useful in improving their confidence in the use of instruments and equipment. This is attributable to the idea that the respondent sees the in-services and training as helpful in reminding them of things they might have forgotten and help them learn new skills.
Participant 4 skipped the question, while Participant 5 explained that the in-service “increases confidence and competency.” Therefore, like Participants 1 and 3, the respondent believes that through in-services, they will be capable of using the instruments and equipment successfully and efficiently. That is, by updating their knowledge and skills, they can use the instruments and equipment confidently.
Both Participants 6 and 13 stated that in-services and training lead to “increased productivity.” Improved productivity means that the respondents agree that by equipping them with new skills, thus preventing them from making mistakes. Increased productivity can also imply that the respondents believe that the acquired skills enable them to efficiently carry out their tasks.
Participants 7 and 12 stated that following the in-services and training, they have witnessed “better performance” or “improved performance.” As highlighted by Participant 5, improved performance could be attributed to “retained skills” which make them more effective in carrying out assigned tasks and using the instruments and equipment. In agreement, Participant 8 stated that training helped them achieve “better outcome and quality service.” The better outcome implies that the training equipped the responded with knowledge, skills, and confidence required to make well-informed diagnoses.
Participant 9 described learning new, advanced medical-surgical technology through in-services as “the best way to learn as you are handling human lives. It helps increase comfortably.” This means that the respondent perceives the in-services as the most effective platform for improving confidence in handling patients. Enhanced confidence is attributed to the participant’s comfort in addressing patients’ needs. Participant 10 just stated that training “helps a lot.” Lastly, Participant 11 emphasized that on-the-job training “is more like a residency. Working hard both with on-the-job training and in-services makes one a competent physician.” Improved competence means that the respondent perceives on-the-job training as crucial in boosting their confidence at work.
To further assess participants’ self-described confidence, they were asked to describe what they believed “would be most effective training process in developing the competency of surgical staff members or in terms of utilizing the new equipment and navigating the technologies inside the operating room.” Participant 1 explained that competency would be best built through “job training.” Specifically, the respondent emphasized that “the most effective training in my experience is on the job training.” Participant 2 did not answer the question. The third respondent agreed with Participant 1 that the most appropriate training is “Hands-on-training, which is mostly acquired with all types of training modes as long as staff members are allowed to work on the instruments and or equipment at the time of training.” Participant 4 skipped the question.
Participant 5 explained that “Most effective training process would be interactive training which simulates realistic scenarios.” Next, Participant 6 emphasized that “Both in-services and on-the-job training” are useful. In agreement, Respondent 7 maintained that “hands-on training” is the best while Participant 8 also agreed that “Hands-on training during either on-the-job or in-services” work the best. Another respondent who agreed that on-the-job training makes them competent were Participants 9 and 10 who described it as “On the job daily training” and “on the job training” respectively. Similarly, Participant 11 and 12 associated competencies with “on the job training is very effective as it is taught by experienced staffer” and “On-the-job training by well-experienced team member” respectively. Lastly, Participant 13 attributed competency to the assumption that “On the job training is better.”
Overall, participants’ responses showed that the most preferred training method is “on-the-job” training (see Figure 5). This may be attributed to the presence of “well-experienced team member” and being “taught by an experienced staffer.” Out of the thirteen participants, six preferred “on-the-job” training. Hands-on-trainings was the second most preferred training method with two respondents supporting it. Similarly, two participants liked “in-services and on-the-job training.” Only one participant preferred “interactive Training/Simulations,” implying that it was not a preferred training method.
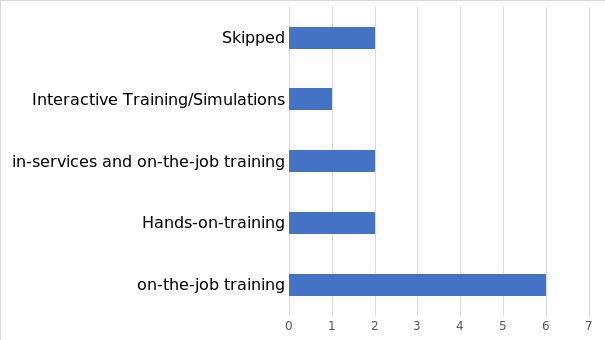
To further understand effective approaches needed to improve staff confidence inside the operating room, the participants were asked to describe “other methods and strategies can be implemented to improve the staff competence and efficiency inside the operating room.” Participant 1 stated that competence and efficiency could be improved through “Pre-recorded video is always useful for playbacks.” In agreement, Participant 3 emphasized that “Prerecorded training” is preferred.
Participant 5 linked improved competence and efficiency to “Teamwork and trust-building activities.” Similarly, Participant 6 seemed to like the idea of teamwork seen through a preference for “Peer training.” According to the seventh respondent, “Daily reminder training before procedures” improves staff confidence in the use of instruments and equipment. Participants 8, 9, and 13 preferred “online training.” Participant 10 wanted “Daily training and in service.” Similarly, the eleventh respondent emphasized on the need for “Daily in-service prior to procedures.” Participant 12 wished for “Daily refresher course before and after each procedure.”
Summary
Conclusively, this chapter presents the findings received as the result of the qualitative descriptive design data analysis. The overall research is aimed at investigating how operating room staff in the northeastern part of the United States learns medical-surgical technology by participating in on-the-job training or in-service training. The analysis of the current research’s findings allowed for answering the stated research questions by means of the questionnaires conducted among surgical room staff. The responses of the sampled population were analyzed, synthesized, and interpreted in accordance with the aims of the research.
In total, thirteen participants participated in this questionnaire, including surgeons, nurses, anesthesiologists, occupational therapists, surgical technologists, and certified registered nurse anesthesiologist. Two participants out of thirteen did not state their current position. Ten participants indicated that they had both on the job training and in-service training, which accounts for 77% of the respondents, while one participant stated that he/she did not participate in any activity, and two skipped this question.
Next, this research aimed to investigate the shortcomings and drawbacks of the technology-related surgical training. Their responses indicate that inadequate curriculum and methodology, as well as having no follow-ups and motivation, are the critical reasons for avoiding professional surgical training. When asked about ways to address these shortcomings, the participants indicated that they would want to have manufacturer’s representatives as instructors, follow up to ensure that the equipment is used appropriately, motivation, and adequate comprehension of the operating room and its dynamics. On the other hand, 23% indicate that rushed training and team disturbance is a major issue during training, while 15% referred to “rushed training” as the main problem.
In the open-ended questions part of the questionnaire, participants were asked to reflect on the ways of improving the current training practices. A participant stated that training sessions should be scheduled in advance to ensure a better turnout. Moreover, this participant complained of having insufficient time to learning new skills. Another participant noted that the trainer should be highly qualified and show competence. Three other participants supported this by arguing that better training for the instructors should be provided prior to the on-the-job training. Finally, distractions, such as socialization between team members, should be minimized as cited by two of the participants.
To reiterate the results, this research found that although the majority of staff members in the operating rooms undergo technology training, there are some significant issues with the way this training is conducted. Despite the shortcomings, 85% agreed that on-the-job training is an effective way of learning new skills required to use advanced surgical technologies. Most participants agreed that such training improves their performance and allows them to have more confidence when working with equipment or instruments in the operating room. On-the-job training was cited by most as the most effective training method. This chapter presents the complete responses of the individuals who participated in the current qualitative descriptive study on education and the use of medical technology.
Conclusions and Recommendations
The current study is designed to investigate the intersection between education and the use of medical technology in the surgical setting. The purpose of the study is to explore the experience of surgical personnel in ambulatory surgical centers in the northeastern part of the United States who learn new, advanced medical-surgical technology through in-services and the acquired level of skill competency. The objective of the current research is to understand how the medical personnel involved in the performance in the operating room perceives the level of their skills in terms of technology usage, as well as their perception of educational forms, techniques, and outcomes as they are used in the modern health care facilities. This final chapter will reiterate research questions to discuss how they were answered. Also, the findings obtained as the result of the conducted qualitative descriptive study will be presented and followed by the discussion of the study’s limitations. Finally, recommendations for leaders and practitioners and implications for future research will be addressed.
Research Questions
For the purposes of qualitative research, the research questions pertinent to the identified topic of education and medical technology use were designed to investigate the ways the studied personnel perceives their experience related to training in technological use. Three research questions were formulated as follows:
- RQ 1: How do surgical personnel describe their experience of learning new, advanced medical-surgical technology through in-services at ambulatory surgical centers in northeastern United States?
- RQ 2: How do surgical personnel at a selected ambulatory surgical centers
- experience in-services as a means to learn to use new, advanced medical-surgical technology ?
- RQ 3: How do surgical personnel describe the effect of learning new, advanced medical-surgical technology through in-services with respect to their self-described confidence in their skill
Discussion of Findings
Overall, 13 participants who represented the members of surgical team responded to the questionnaire investigating their experience in training, perception of the outcomes and the reasons for drawbacks. The findings of the study might be grouped in several sections.
Shortcomings and Drawbacks of In-Service Training Strategies
The study identified that the major reasons for drawbacks in the effectiveness of in-service training they attended were of internal and external nature. Firstly, the key factor in the diminished effectiveness of in-service training strategies is the inappropriate methodology and curriculum. Another reason, as perceived by the participants, is the lack of follow-up activities and insufficient motivation. These findings are consistent with those obtained by Bahler and Sundaram (2014) who found well-structured curriculum one of the core elements in achieving positive results in robotic surgery training. As perceived by the personnel, the best ways to address the identified shortcomings include manufacturers’ representatives as trainers, motivation and interactive instruction, follow-ups, and adequacy of trainers.
Shortcomings and Drawbacks of On-the-Job Training Strategies
The findings demonstrated that the frequently observed drawbacks and shortcomings in the implementation of on-the-job training for surgeons were determined by ineffective trainers, team disturbances, rushed training, and low productivity. These findings match the previous studies results but contribute to the scope of literature by identifying more reasons of possible inadequacy of training techniques. For example, the importance of effective trainers especially in the surgical setting expands the findings of Bamford and Coulston (2016). As the ways of addressing these shortcomings, the participants identified timely training by qualified staff and minimizing distractions as the most important ones.
Participants’ Experience and Confidence
Despite the identified difficulties with the effectiveness and feasibility of training interventions, the majority of participants admitted the usefulness and overall positive effect of training on their level of skills of technological use. It implies that once addressed from the perspective of the proposed improvements, the training strategies applicable to surgical team’s utilization of technologies will deliver better practical outcomes. The increased level of knowledge and competence in using advanced technologies in the operating room has amplified the personnel’s confidence and contributed to the safety of patients. These findings agree with and contribute to those of Cavalini (2014) and Cervantes-Sanchez (2015).
Limitations
The limitations of the study are those related to the population and the chosen study design. Firstly, the sampled participants’s diversity is not perfectly distributed across the team roles. The number of CRNAs and occupational therapists was less than that of other team representatives. Also, the subjective nature of the study that is limited to the interpretation of the data by the participants might be considered a limitation. Since the perceived attitudes dominated in responses, the findings of the research are influenced by the subjective views of the personnel.
Recommendations to Leaders and Practitioners
Since the problem addressed in this study is the lack of understanding the experience of medical personnel engaged in training for technology use, the study findings might be helpful in filling this gap and solving this problem. The leaders of health care facilities might construct better training sessions, employ more qualified experts and trainers who would lead the learning process effectively. Since one of the reported problems was the lack of motivation, leaders should implement benefits for personnel who attend training and demonstrate positive results. As for the practitioners, it is recommended to expand their knowledge and skills within the realm of technological advancement by means of systematic attending of training sessions, stimulating inner motivation for professional development, and allocation of sufficient time and resources for continuous learning.
Recommendations for Future Research
The conducted research might serve as a solid ground for future research. Since the field of technology use training in the surgical domain is relatively scarce, extensive investigation of the issues related to the topic are encouraged. The current qualitative descriptive study has presented an observational data concerning the most frequently observed problems in effectiveness of training strategies. Future research should concentrate on specific problems and reasons. Also, it is encouraged to utilize experimental and quantitative methodologies to diversify the scope of findings and improve the quality of training in the medical setting.
Conclusion
In summation, the study investigated how the education and medical technology intersect in the surgical setting as perceived by the members of operating room team. The questions that were aimed to be answered in the course of the study included How do surgical personnel describe their experience of learning new, advanced medical-surgical technology through in-services at ambulatory surgical centers in northeastern United States? How do surgical personnel at a selected ambulatory surgical centers experience in-services as a means to learn to use new, advanced medical-surgical technology ? How do surgical personnel describe the effect of learning new, advanced medical-surgical technology through in-services with respect to their self-described confidence in their skill?
The findings demonstrate that despite the overall perceived effectiveness of in-service and on-the-job training, the participants reported significant problems that caused drawbacks and shortcomings in learning. They include inappropriate methodology and curriculum, the lack of follow-up activities and insufficient motivation, ineffective trainers, team disturbances, rushed training, and low productivity. However, the proposed ways to address these problematic areas are feasible and should be implemented in practical settings. The findings optimistically contribute to the scope of current literature and provide a solid background for future research. The description of the drawbacks and their elimination will be valuable information for leaders and practitioners working in surgical settings using advanced technology.
References
Acton, A. (2013a). Issues in surgical research, techniques, and innovation. (Scholarly brief]. Scholarly Editions.
Acton, A. (2013b). Minimally invasive surgical procedures—Advances in research and application. (Scholarly brief). Scholarly Editions.
Aho, J. M., Ruparel, R. K., Graham, E., Zendejas-Mummert, B., Heller, S. F., Farley, D. R., & Bingener, J. (2015). Mentor-guided self-directed learning affects resident practice. Journal of surgical education, 72, 674-679. Web.
Alfredson, H., & Isaksson, M. (2014). Ultrasound and color doppler-guided surgery for insertional Achilles tendinopathy-results of a pilot study. Open Journal of Orthopedics, 4, 7-14. Web.
Angus, A. A., Sahi, S. L., & McIntosh, B. B. (2014). Learning curve and early clinical outcomes for a robotic surgery novice performing robotic single site cholecystectomy. International Journal of Medical Robotics, 10, 203-207. Web.
Arakelian, E., Gunningberg, L., & Larsson, J. (2011). How operating room efficiency is understood in a surgical team: A qualitative study. International Journal for Quality in Health Care, 23(1), 100-106. Web.
Arunachalam, S., & Ansell, J. (2017). The use of simulation training for robotic-assisted surgery. Journal of Surgical Simulation, 4, 48-51. Web.
Association of American Medical Colleges. (n.d.). Policy priorities to improve our nation’s health: How medical education is changing. Association of American Medical Colleges. Web.
Bach, C., Miernik, A., & Schnthaler, M. (2014). Training in robotics: The learning curve and contemporary concepts in training. Arab Journal of Urology, 12(1), 58-61. Web.
Badash, I., Burtt, K., Solorzano, C. A., & Carey, J. N. (2016). Innovations in surgery simulation: A review of past, current, and future technologies. Annals of Translational Medicine, 4(23), 453. Web.
Bahler, C. D., & Sundaram, C. P. (2014). Training in robotic surgery: Simulators, surgery, and credentialing. Urologic Clinics, 41(4), 581-589. Web.
Bamford, R., & Coulston, J. (2016). Effective e-learning in surgical education: The core values underpinning effective e-learning environments and how these may be enhanced for future surgical education. Ecancermedicalscience, 10(ed13). Web.
Barrie, J., Jayne, D. G., Wright, J., Murray, C. J., Collinson, F. J., & Pavitt, S. H. (2014). Attaining surgical competency and its implications in surgical clinical trial design: A systematic review of the learning curve in laparoscopic and robot-assisted laparoscopic colorectal cancer surgery. Annual Surgical Oncology, 21, 829-840. Web.
Basodogan, C., De, S., Kim, J., Muniyandi, M., Kim, H., & Srinivasan, M. A. (2004). Haptics in minimally invasive surgical simulation and training. IEEE Computer Graphics and Applications, 24(2), 56-64. Web.
Benmessaoud, C., Kharrazi, H., & MacDorman, K. F. (2011). Facilitators and barriers to adopting robotic-assisted surgery: Contextualizing the unified theory of acceptance and use of technology. PLoS One, 6(1), e16395. Web.
Berg, B. L. (2006). Qualitative research methods for the social sciences (6th ed.). Pearson/Allyn & Bacon.
Boone, B. A., Zenati, M., Hogg, M. E., Steve, J., Moser, A., Bartlett, D. L., Zeh, H. J. Zureikar, A. H. (2015). Assessment of quality outcomes for robotic pancreaticoduodenectomy: Identification of the learning curve. Journal of the American Medical Association, 150, 416-422. Web.
Carter, S. C., Chiang, A., Shah, G., Kwan, L., Montgomery, J. S., Karam, A., Tarnay, C., Guru, K.A., & G., Hu, J. C. (2015). Video-based peer feedback through social networking for robotic surgery simulation: A multicenter randomized controlled trial. Anal Surgery, 261, 870-875. Web.
Catchpole, K., Perkins, C., Bresee, C., Solnik, M. J., Sherman, B., Fritch, J., Gross, B., Jagannathan, S., Hakami-Majd, N., Avenido, R., & Anger, J. T. (2016). Safety, efficiency, and learning curves in robotic surgery: A human factors analysis. Surgery Endoscopy, 30, 3749-3761. Web.
Cavalini, W. L. P., Claus, C. M. P., Dimbarre, D., Cury Filho, A. M. C., Bonin, E. A., Loureiro, M. P., & Salvalaggio, P. (2014). Development of laparoscopic skills in medical students naïve to surgical training. Einstein (San Paulo), 12(4), 467-472. Web.
Cervantes-Sanchez, C. R., Chavez-Vizcarra, P., Barragan-Avila, M. C., Acosta, H. P., & Herrera-Mendoza, R. E. (2015). What and how to evaluate clinical-surgical competence. The resident and staff surgeon perspective. Cirugia y Cirujanos, 84(4), 301-308. Web.
Champagne, B. J. (2013). Effective teaching and feedback strategies in the operating room and beyond. Clinics in Colon and Rectal Surgery, 26(4), 244–249. Web.
Chang, L., Satava, R. M., Pellegrini, C. A., & Sinanan, M. N. (2003). Robotic surgery: Identifying the learning curve through objective measurement of skill. Surgical Endoscopy and Other Interventional Techniques, 17(11), 1744-1748. Web.
Chen, R. F., & Hsiao, J. L. (2012). An investigation on physicians’ acceptance of hospital information systems: A case study. International Journal of Medical Informatics, 81(12), 810-820. Web.
Cristancho, S. M., Goldszmidt, M., Lingard, L., & Watling, C. (2018). Qualitative research essentials for medical education. Singapore Medical Journal, 59(12), 622–627. Web.
Christensen, C. (2013). The innovator’s dilemma: When new technologies cause great firms to fail. Harvard Business Review Press.
Clifton, M. S., & Wulkan, M. L. (2015). Innovation in pediatric surgical education. Seminars in Pediatric Surgery, 24(3), 122-123. Web.
Covens, A., Kohler, C., Joo-Hyun, N., Naumann, R. W., Obermair, A., & Querleu, D. (2016). Cost-efficiency of robotic surgery. International Journal of Gynecological Cancer, 26(6), 992-993. Web.
Courteau, B. C., Knox, A., Vassiliou, M. C., Warren, R. J., & Gilardino, M. S. (2015). The development of assessment tools for plastic surgery competencies. The Aesthetic Surgery Journal, 35(5), 611-617. Web.
Cullinan, D. R., Wise, P. E., Delman, K. A., Potts, J. R., Awad, M. M., Eberlein, T. J., & Klingensmith, M. E., (2018). Interim analysis of a prospective multi-institutional study of surgery resident experience with flexibility in surgical training. Journal of the American College of Surgeons, 226, 425-431. Web.
da Cruz, J. A. S., dos Reis, S. T., Cunha Frati, R. M. C., Duarte, R. J., Nguyen, H., Srougi, M., & Passerotti, C. C. (2016). Does warm-up training in a virtual realty simulator improve surgical performance? A prospective randomized analysis. Journal of Surgical Education, 73, 974-978. Web.
Davis, F. D. (1989). Perceived usefulness, perceived ease of use, and user acceptance of information technology. MIS Quarterly, 13, 319-340. Web.
Dawe, S. R., Windsor, J. A., Broeders, J. A., Cregan, P. C., Hewett, P. J., & Maddern, G. J. (2014). A systematic review of surgical skills transfer after simulation-based training: Laparoscopic cholecystectomy and endoscopy. Annals of Surgery, 259, 236-248. Web.
Denzin, N. K., & Lincoln, Y. S. (Eds.). (2017). Introduction: The discipline and practice of qualitative research. In N. K. Denzin & Y. S. Lincoln (Eds.), Sage handbook of qualitative research (5th ed., pp. 1–42). Sage.
Deutsch, G. B., Sathyanarayana, S. A., Giangola, M., Akeman, M., DeNoto, G., III, Klein, J. D., Zemon, H., & Rubach, E. (2015). Competence acquisition for single-incision laparoscopic cholecystectomy. Journal of the Society of Laparoendoscopic Surgeons, 19(1), e2014-00116. Web.
Dubé, C., & Rostom, A. (2016). Acquiring and maintaining competency in gastrointestinal endoscopy. Best Practice & Research Clinical Gastroenterology, 30, 339-347. Web.
Egeland, R. D., Rapp, Z., & David, F. S. (2017). From innovation to market adoption in the operating room: The “CFO as customer.” Journal of Surgery; Open Access, 162, 477-482. Web.
Einarsson, J. (2014). Operating room: Robotic surgery has no advantages over conventional laparoscopic surgery. Royal College of Obstetricians and Gynecologists,121(12), 1554. Web.
Ekkelenkamp, V. E., Koch, A. D., de Man, R. A., & Kuipers, E. J. (2016). Training and competence assessment in GI endoscopy: A systematic review. Gut, 65(4), 607-615. Web.
El Bardissi, A. W., & Sundt, T. M. (2012). Human factors and operating room safety. Surgical Clinics of North America, 92(1), 21-35. Web.
Entezami, P., Franzblau, L. E., & Chung, K. C. (2012). Mentorship in surgical training: A systematic review. Hand, 7(1), 30-36. Web.
Eshun, P., & Eshun, N. (2013). Attitudes of perioperative personnel: A comparative research on safety culture and usage of surgical safety checklist [Doctoral dissertation]. Web.
Evans, C. H., & Schenarts, K. D. (2016). Evolving educational techniques in surgical training. Surgical Clinician North America, 96(1), 71-88. Web.
Fard, M. J., Ameri, S., Chinnam, R. B., Pandya, A. K., Klein, M. D., & Ellis, R. D. (2016). Machine learning approach for skill evaluation in robotic-assisted surgery. Web.
Forse, R. A., Bramble, J. D., & McQuillan, R. (2011). Team training can improve operating room performance. Surgery, 150(4), 771-778. Web.
Gallivan, M. J. (1997). Value in triangulation: A comparison of two approaches for combining qualitative and quantitative methods. In A. S. Lee, J. Liebenau, & J. J. DeGross (Eds.). Information systems and qualitative research (pp. 417-443). Springer. Web.
Gaitanidis, A., Simopoulos, C., & Pitiakoudis, M. (2018). What to consider when designing a laparoscopic colorectal training curriculum: A review of the literature. Techniques in Coloproctology, 22(3), 151-160. Web.
Gallagher, A. G., O’Sullivan, G. C., & Traynor, O. (2014). An objective evaluation of a multi-component, competitive, selection process for admitting surgeons into higher surgical training in a national setting. World Journal of Surgery, 38(2), 296-304. Web.
Gay, L. R., Mills, G. E., & Airasian, P. (2006). Educational research: Competencies for analysis and applications (8th ed.). Pearson-Merrill Prentice Hall.
Gearhart, S. L., Wang, M. H., Gilson, M. M., Chen, B., & Kern, D. E. (2012). Teaching and assessing technical proficiency in surgical subspecialty fellowships. Journal of Surgical Education, 69(4), 521-528. Web.
Gordon, M., Darbyshire, D., & Baker, P. (2012). Non‐technical skills training to enhance patient safety: A systematic review. Medical Education, 46, 1042-1054. Web.
Groenier, M., Groenier, K. H., Miedema, H. A., & Broeders, I. A. (2015). Perceptual speed and psychomotor ability predict laparoscopic skill acquisition on a simulator. Journal of surgical education, 72(6), 1224-1232. Web.
Groenwald, T. (2004). A phenomenological research design illustrated. International Journal of Qualitative Methods, 3, 1-12. Web.
Gross, N. D., Holsinger, F. C., Magnuson, J. S., Duvvuri, U., Genden, E. M., Ghanem, T. A., Yaremchuk, K. L., Goldenberg, D., Miller, M. C., Moore, E. J., Morris, L. G., Netterville, J., Weinstein, G. S., & Richmon, J. (2016). Robotics in otolaryngology and head and neck surgery: Recommendations for training and credentialing: A report of the 2015 AHNS Education Committee, AAO-HNS Robotic Task Force, and AAO-HNS Sleep Disorders Committee. Head & Neck, 38(1), 151-158. Web.
Grover, A., Orlowski, J. M., & Erikson, C. E. (2016). The nation’s physician workforce and future challenges. Improving U.S. Healthcare Symposium, 351(1), 11-19. Web.
Guba, E. G., & Lincoln, Y. S. (2005). Paradigmatic controversies, contradictions, and emerging confluences. In N. K. Denzin & Y. S. Lincoln (Eds.), Sage handbook of qualitative research (3rd ed., pp. 191–215). Sage.
Guend, H., Widmar, M., Patel, S., Nash, G. M., Paty, P. B., Guillem, J. G., Temple, L. K., Garcia-Aguilar. J., & Weiser, M. R. (2017). Developing a robotic colorectal cancer surgery program: Understanding institutional and individual learning curves. Surgical Endoscopy, 31, 2820-2828. Web.
Hall, M. J., Schwartzman, A., Zhang, J., & Liu, X. (2017). Ambulatory surgery data from hospitals and ambulatory surgery centers: United States, 2010. National health statistics reports, (102), 1. Web.
Harrysson, I. J., Cook, J., Sirimanna, P., Feldman, L. S., Darzi, A., & Aggarwal, R. (2014). Systematic review of learning curves for minimally invasive abdominal surgery: A review of the methodology of data collection, depiction of outcomes, and statistical analysis. Annals of Surgery, 260(1), 37-45. Web.
Harrysson, I. J., Hull, L., Sevdalis, N., Darzi, A., & Aggarwal, R. (2014). Development of a knowledge, skills, and attitudes framework for training in laparoscopic cholecystectomy. The American Journal of Surgery, 207, 790-796. Web.
Healy, J. M., Maxfield, M. W., Solomon, D. G., Longo, W. E., & Yoo, P. S. (2018). Beyond 250: A comprehensive strategy to maximize the operative experience for junior residents. Journal of Surgical Education, 75(3), 1-5. Web.
Hein, S. F., & Austin, W. J. (2001). Empirical and hermeneutic approaches to phenomenological research in psychology: A comparison. Psychological Methods, 6, 3-17. Web.
Herrell, S. D., & Smith, J. A. (2005). Robotic-assisted laparoscopic prostatectomy: What is the learning curve? Urology, 66(5), 105-107. Web.
Honaker, M. D., Paton, B. L., Stefanidis, D., & Schiffern, L. M. (2015). Can robotic surgery be done efficiently while training residents? Journal of Surgical Education, 72(3), 377-380. Web.
Huber, T., Passholder, M., Hansen, C., Wondering, T., Lang, H., & Kneist, W. (2017). New dimensions in surgical training: Immersive virtual reality laparoscopic simulation exhilarates surgical staff. Surgical Endoscopy, 31, 4472-4477. Web.
Jaffe, T. A., Hasday, S. J., Knol, M., Pradarelli, J., Quamme, S. R. P., Greenberg, C. C., & Dimick, J. B. (2017). Strategies for new skill acquisition by practicing surgeons. Journal of Surgical Education, 75, 928-934. Web.
Jang, S. W., Ko, J., Choi, Y. J., & Kim, Y. S. (2017). A development of an epiduroscopy training simulator based on spatial cognition learning. Journal of Vibroengineering PROCEDIA, 14, 250-255. Web.
Jeanfreau, S. G., & Jack, L., Jr. (2010). Appraising qualitative research in health education: Guidelines for public health educators. Health Promotion Journal, 11, 612–617. Web.
Jeppson, P. C., Rahimi, S., Gattoc, L., Westermann, L. B., Cichowski, S., Raker, C., Weber Lebrun, E. E., & Sung, V.W. (2015). Impact of robotic technology on hysterectomy route and associated implications for resident education. American Journal of Obstetrics and Gynecology, 212, 196e1-196e6. Web.
Jones, D. B., Sung, R., Weinberg, C., Korelitz, T., & Andrews, R. (2016). Three-dimensional modeling may improve surgical education and clinical practice. Surgical Innovation, 23(2), 189-195. Web.
Juanes, J. A., Gomez, J. J., Peguero, P. D., & Ruisoto, P. (2016). Digital environment for
movement control in surgical skill training. Journal of Medical System, 40(6), 133. Web.
Karmali, D. J. (2017). Heated insufflation with or without humidication for laparoscopic abdominal surgery. A Cochrane Database of Systematic Reviews, 1(1), 12. Web.
Khan, N., Abboudi, H., Khan, M. S., Dasgupta, P., & Ahmed, K. (2014). Measuring the surgical “learning curve”: Methods, variables, and competency. British Journal of Urology International, 113, 504-508. Web.
Khor, W., S., Baker, B., Amin, K., Chan, A. Patel, K., & Wong, J. (2016). Augmented and virtual reality in surgery–the digital surgical environment: Applications, limitations and legal pitfalls. Annals of Translational Medicine, 4, 454. Web.
Knowles, M. S., Holton, E. F., III, & Swanson, R. A. (2015). The adult learner: The definitive classic in adult education and human resource development (6th ed.). Elsevier.
Lamb, M. N., & Bardakcioglu, O. (2017). The learning curve of robotic-assisted laparoscopic colorectal surgery and how to start applying robotic technology in colorectal surgery. Robotic Colon and Rectal Surgery, 11-15. Web.
Lenihan, J. P., Kovanda, C., & Seshadri-Kreaden, U. (2008). What is the learning curve for robotic-assisted gynecologic surgery? Journal of Minimally Invasive Gynecology, 15, 589-594. Web.
Lillemoe, K. D., Klingensmith, M. E., Darzi, A., & Taylor, S. M. (2017). American surgical association presidential forum: A lifetime of surgical education-can we do better? Annals of Surgery, 266, 555-563. Web.
Lincoln, Y. S., & Guba, E. G. (1985). Naturalistic inquiry. Sage.
Livinti, I., Osofsky, R., Burgamy, A., Loehrke-Sichhart, L., Mikhail, M., & Shah, A.J. (2015). Laparoscopic versus robotic surgery learning curves. The Journal of Minimally Invasive Gynecology, 22(6), S8-S9. Web.
Machtmes, K., Johnson, E., Fox, J., Burke, M. S., Harper, J., Arcemont, L., Hebert, L., Tarifa, T., Brooks, R. C., Jr., Reynaud, A. L., Deggs, D., Matzke, B., & Aguirre, R. T. P. (2009). Teaching qualitative research methods through service-learning. The Qualitative Report, 14(1), 155–164. Web.
Maertens, H., Madani, A., Landry, T., Vermassen, F., Herzeele, V., & Aggarwal, R. (2016). Systematic review of e-learning for surgical training. British Journal of Surgery, 103, 1428-1437. Web.
Maier-Hein, L., Vedula, S., Speidel, S., Navab, N., Kikinis, R., Park, A., Eisenmann, M., Feussner, H., Foretier, G., Giannarou, S., Hashizume, M., Katic, D., Kenngott, H., Kranzfelder, A. M., Mäwz, K., Neumuth, T., Padoy, N., Pugh, C., Schoch, N., Stoyanov, D., & Janin, P. (2016). Surgical data science: Enabling next-generation surgery. Web.
Maillet, É., Mathieu, L., & Sicotte, C. (2015). Modeling factors explaining the acceptance, actual use and satisfaction of nurses using an Electronic Patient Record in acute care settings: An extension of the UTAUT. International Journal of Medical Informatics, 84(1), 36-47. Web.
Manuel-Palazuelos, J. C., Riano-Molleda, M., Ruiz-Gomez, J. L., Martin-Parra, J. I., Redondo-Figuero, C., & Maestre, J. M. (2016). Learning curve patterns generated by training method for laparoscopic small bowel anastomosis. Advances in Simulation, 1(16), 1-10. Web.
Matern, U., & Koneczny, S. (2007). Safety, hazards and ergonomics in the operating room. Surgical Endoscopy, 21, 1965-1969. Web.
Maxwell, J. A. (2004). Qualitative research design: An interactive approach (2nd ed.) Sage.
McGaghie, W. C., Issenberg, S. B., Barsuk, J. H., & Wayne, D. B. (2014). A critical review of simulation-based learning with translational outcomes. Medical Education, 48, 375- 385. Web.
McLaughlin, M. M. (2012). A model to evaluate efficiency in operating room processes [Doctoral dissertation]. University of Michigan, Dearborn, MI. Web.
Merali, N., Veeramootoo, D., & Singh, S. (2017). Eye-tracking technology in surgical training. Journal of Investigative Surgery, 1-7.
Merriam, S. B. (2001). Andragogy and self-directed learning: Pillars of adult learning theory. New Direction for Adult and Continuing Education, 89, 3-13. Web.
Merriam, S. B., Caffarella, R. S., & Baumgartner, L. M. (2012). Learning in adulthood: A comprehensive guide (3rd ed.). Jossey-Bass.
Mertler, C. A., & Charles, C. M. (2006). Introduction to educational research (6th ed.). Pearson Allyn & Bacon.
Moore, L. J., Wilson, M. R., Waine, E., Masters, R. S., McGrath, J. S., & Vine, S. J. (2015). Robotic technology results in faster and more robust surgical skill acquisition than traditional laparoscopy. Journal of Robotic Surgery, 9(1), 67-73. Web.
Moriates, C., Dohan, D., Spetz, J., & Sawaya, G. (2015). Defining competencies for education in health care value. Academic Medicine, 90, 421-424. Web.
Morgan, R. (2014). Smart surgery–a new era in surgical technology: Recent advances and future trends. Academic Medicine, 190(4), 21. Web.
Moustakas, C. (1994). Phenomenological research methods. Sage.
Nemani, A., Ahn, W., Cooper, C., Schwaitzberg, S., & De, S. (2018). Convergent validation and transfer of learning studies of a virtual reality-based pattern-cutting simulator. Surgical Endoscopy, 32(3), 1265-1272. Web.
Nemani, V. M., Park, C., & Nawabi, D. H. (2014). What makes a “great resident”: The resident perspective. Curriculum Review Muscoloskeletal Medicine, 7, 164-165. Web.
Ozuah, P. O. (2016). First, there was pedagogy and then came andragogy. Einstein Journal of Biology and Medicine, 21(2), 83-87. Web.
Panait, L., Shetty, S., Shewokis, P. A., & Sanchez, J. A. (2014). Do laparoscopic skills transfer to robotic surgery? Journal of Surgical Research, 187(1), 53-58. Web.
Papachristofi, O., Jenkins, D., & Sharples, L. D. (2016). Assessment of learning curves in complex surgical interventions: A consecutive case-series study. Trials, 17, 266. Web.
Patton, M. Q. (1987). How to use qualitative methods in evaluation (2nd ed.). Sage.
Patton, M. Q. (2001). Qualitative research and evaluation methods (3rd ed.). Sage.
Patton, M. Q., & Cochran, M. (2002). A guide to using qualitative research methodology. Sage.
Patel, V., Aggarwal, R., Osinibi, E., & Darzi, A. (2012). Operating room introduction for the novice. The American Journal of Surgery, 203(2), 266-275. Web.
Pedowitz, R. A. (2017). Virtual reality surgical simulation for arthroscopy training. Journal of Medical Education and Training, 1, 8. Web.
Perino, A., Cucinella, G., Venezia, R., Castelli, A., & Cittadini, E. (1999). Total laparoscopic hysterectomy versus total abdominal hysterectomy: An assessment of the learning curve in a prospective randomized study. Human Reproduction, 14, 2996-2999. Web.
Phillips, N. (2013). Berry & Kohn’s operating room technique. Elsevier Health Sciences.
Polkinghorne, D. E. (1989). Phenomenological research methods. In R. S. Valle & S. Halling (Eds.), Existential-phenomenological perspectives in psychology: Exploring the breadth of human existence (pp. 41–62). Plenum.
Rashid, P. (2017). Surgical education and adult learning: Integrating theory into practice. F1000Research, 6. Web.
Ridley, D. (2012). The literature review: A step-by-step guide for students. Sage.
Roberts, K. E., Bell, R. L., & Duffy, A. J. (2006). Evolution of surgical skills training. World Journal of Gastroenterology, 12, 3219. Web.
Romeo, A. A. (2016). Surgical skill education: Deficiency in the learning curve has to change. Orthopedics Today [online]. Web.
Ryan, F., Coughlan, M., & Cronin, P. (2007). Step-by-step guide to critiquing research. British Journal of Nursing, 16, 738-744. Web.
Sadideen, H., Alvand, A., Saadeddin, M., & Kneebone, R. (2013). Surgical experts: Born or made? International Journal of Surgery, 11, 773-778. Web.
Sanchez-Peralta, L. F., Sanchez-Fernandez, J., Pagador, J. B., & Sanchez-Margallo, F. M. (2013). New technologies in minimally invasive surgery training: What do surgeons demand? Cirugia y Cirujanos [Surgery and Surgeons], 81, 412-419. Web.
Sears, K., Godfrey, C., Luctkar, M. F., Ginsburg, L., Tregunno, D., & Ross-White, A. (2014). Measuring competence in health care learners and health care professionals by comparing self-assessment with objective structured clinical examinations (OSCEs): A systematic review protocol. JBI Database of Systematic Reviews and Implementation Reports, 12(3), 24-38. Web.
Sharma, V., Surek, C., Stewart, H., Stephens, R., & Wright, B. (2016). Integrating surgical skills into pre-clinical years of medical school. Journal of Surgery: Open Access, 2(3), 1-21. Web.
Shenton, A. K. (2004). Strategies for ensuring trustworthiness in qualitative research projects. Education for Information, 22, 63-75. Web.
Simon, M. K. (2006). Dissertations and scholarly research: Recipes for success. Kendall/Hunt.
Smith, J. A., Flowers, P., & Larkin, M. (2009). Interpretative phenomenological analysis: Theory, method, and research. Sage.
Smith, R. D. (2009). Investigating the disruptive effect of computer game technologies on medical education and training [Doctoral dissertation]. University of Maryland University College. Web.
Smyth, J. K., Deveney, K., & Sade, R. M. (2013). Who should adopt robotic surgery, and when? The Annals of Thoracic Surgery, 96(4), 1-8. Web.
Sood, A., Jeong, W., Ahlawat, R., Campbell, L., Aggarwal, S., Menon, M., & Bhandari, M. (2015). Robotic surgical skill acquisition: What one needs to know? Journal of Minimal Access Surgery, 11(1), 10-15. Web.
Spruit, E. N., Band, G. P. H., & Hamming, J. F. (2014). Increasing efficiency of surgical training: Effects of spacing practice on skill acquisition and retention in laparoscopy training. Surgical Endoscopy, 8, 2235-2243. Web.
Sridhar, A. N., Briggs. T. P., Kelly, J. D., & Nathan, S. (2017). Training in robotic surgery–An overview. Curriculum Urology Reports, 18(58), 1-8. Web.
Stanford, S. B., Lee, S., Masaquel, C., & Lee, R. H. (2015). Achieving competence in colonoscopy: Milestones and the need for a new endoscopic curriculum in gastroenterology training. World Journal of Gastrointestinal Endoscopy, 7, 1279. Web.
Stefanidis, D., Scerbo, M. W., Montero, P. N., & Smith, W. D. (2012). Simulator training to automaticity leads to improved skill transfer compared with traditional proficiency-based training: A randomized controlled trial. Annals of Surgery, 255(1), 30-37. Web.
Subramonian, K., & Muir, G. (2004). The “learning curve” in surgery: What is it, how do we measure it and can we influence it? British Journal of Urology International, 93(9), 1173-1174. Web.
Swain, J. D., Matousek, A. C., Scott, J. W., Cooper, Z., Smink, D. S., Bolman, R. M., III, Finlayson, S. R. G., Zinner, M. J., & Riviello, R. (2015). Training surgical residents for a career in academic global surgery: A novel training model. Global Health Initiatives, 72(4), 104-110. Web.
Tassios, P. S., Ladas, S. D., Grammenos, I., Demertzis, K., & Raptis, S. A. (1999). Acquisition of competence in colonoscopy: The learning curve of trainees. Endoscopy, 31, 702-706. Web.
Tomlin, Z., Humphrey, C., & Rogers, S. (1999). General practitioners’ perceptions of effective health care. British Medical Journal, 318, 1532-1535. Web.
Ulrich, B., & Kear, T. (2014). Patient safety and patient safety culture: Foundations of excellent health care delivery. Nephrology Nursing Journal, 41(5), 447-505. Web.
Usher, R., & Bryant, I. (2014). Adult education as theory, practice and research: The captive triangle. Routledge.
Vagle, M. D. (2009). Validity as intended: “Bursting forth toward” bridling in phenomenological research. International Journal of Qualitative Studies in Education, 22, 585–605. Web.
Valente, D. S., Eifler, L. S., Carvalho, L. A., Filho, G. A. P., Ribeiro, V.W., & Padoin, A. V. (2015). Telemedicine and plastic surgery: A pilot study. Plastic Surgery International, 1-4. Web.
Vavra, P., Roman, J., Zonča, P., Ihnát, P., Němec, M., Kumar, J., Habib, N., & El-Gendi, A. (2017). Recent development of augmented reality in surgery: A review. Journal of Healthcare Engineering, 1-9. Web.
Venkatesh, V. (2000). Determinants of perceived ease of use: Integrating control, intrinsic motivation, and emotion into the technology acceptance model. Information Systems Research, 11, 342-365. Web.
Venkatesh, V., & Davis, F. D. (2000). A theoretical extension of the technology acceptance model: Four longitudinal field studies. Management Science, 46, 186-204. Web.
Venkatesh, V., Morris, M. G., Davis, G. B., & Davis, F. D. (2003). User acceptance of information technology: Toward a unified view. MIS Quarterly, 27, 425-478. Web.
Vera, A. M., Russo, M., Mohsin, A., & Tsuda, S. (2014). Augmented reality telementoring (ART) platform: A randomized controlled trial to assess the efficacy of a new surgical education technology. Surgical Endoscopy, 28, 3467-3672. Web.
Vickers, A. J. (2013). What are the implications of the surgical learning curve? European Association of Urology, 65, 523-533. Web.
Waltzman, J. T., Tadisina, K. K., & Zins, J. E. (2014). The rise of technology in plastic surgery education: Is the textbook dead on arrival (DOA)? The Aesthetic Surgery Education and Research Foundation, 36(2), 237-243. Web.
Waring, J., & Bishop, S. (2015). George Ritzer: Rationalization, consumerism and the medialization of surgery. In F. Colyer (Ed.), The Palgrave handbook of social theory in health, illness and medicine (pp. 488-503). Palgrave Macmillan.
Whitfield, N. (2015). Surgical skills beyond scientific management. Medical history, 59, 421-442. Web.
Whittemore, R., Chase, S. K., & Mandle, C. L. (2001). Pearls, pith and provocation: Validity in qualitative research. Qualitative Health Research, 11(4), 522-537. Web.
World Health Organization (WHO). (2010). Increasing complexity of medical technology and consequences for training and outcome of care. (Background paper 4). Web.
Yin, R. K. (2017). Case study research and applications: Design and methods. Sage.
Zendajas, B., Wang, A. T., Brydges, R., Hamstra, S. J., & Cook, D. A. (2013). Cost: The missing outcome in simulation-based medical education research: A systematic review. Surgery, 153, 160-176. Web.
Appendix A
Informed Consent
Greetings,
My name is Student and I am a student at the University of Lancaster working on Doctor of Education in Educational Leadership with a specialization in Educational Technology. I am conducting a research study entitled Education and the Use of Medical Technology: A Qualitative Descriptive Study.
The purpose of the research study is to understand the experience of surgical personnel in ambulatory surgical centers in northeastern part of the United States who learn new, advanced medical-surgical technology through in-services and on-the-job training. This is to learn how surgical personnel perceive their skill level or competency with medical-surgical technology following these types of trainings.
Findings from this study may shed light on the means of enhancing knowledge and skill acquisition regarding the use of modern technology. Participants may gain insight to the most effective training approach in operating room which may improve performance of surgical staff resulting in benefits to surgical patients as success rates in surgical procedures increase because of an effective training approach.
Your participation will involve completing a web-based questionnaire available on any computer by logging in to SurveyMonkey website. You will review and accept the terms of consent. If you agree to the term of the informed consent form, you will be prompted to continue with the questionnaire. If you do not agree with the terms of the informed consent form, you will not be able to proceed with the questionnaire.
- Time commitment for the questionnaire is between 20 to 30 mins.
- All names or identifiers will be removed during the analysis and presentation of data by SurveyMonkey personnel. Before proceeding to the questionnaire, participants will be asked to agree to the terms the informed consent in order to be able to proceed. If a participant does not agree to the terms of the informed consent form, the participant will not be able to proceed. If participants decide to withdraw, their respective data will be removed from the database as they log off the website.
You can decide to be a part of this study or not. Once you start, you can withdraw from the study at any time without any repercussions. The results of the research study may be published but your identity will remain anonymous, and your name will not be made known to any outside parties.
In this research, there are no foreseeable risks to you, but you may be exposed to any risk associated with completing an online survey, which may be a risk of being susceptible to online virus that may invade your computer. It is highly recommended that you install virus protection on your computer.
Although there may be no direct benefit to you, a possible benefit from your being part of this study is that the study may shed light on the means of enhancing knowledge and skill acquisition regarding the use of the modern technology. Participants may gain insight to the most effective training approach in operating room which may improve performance of surgical staff resulting in benefits to surgical patients as success rates in surgical procedures increase because of an effective training approach.
If you have any questions about the research study, please call me or email me. For questions about your rights as a study participant, or any concerns or complaints, please contact the University of Lancaster Institutional Review Board.
As a participant in this study, you should understand the following:
- You may decide not to be part of this study or you may want to withdraw from the study at any time while filling out the questionnaire online by logging off the site. All submitted questionnaire will be final and will be anonymous.
- Your identity will be kept anonymous.
- Student, the researcher, has fully explained the nature of the research study and has answered all of your questions and concerns.
- Data will be kept secure by keeping it in a locked file drawer in home office to which only the researcher has access. The data will be kept for three (3) years, and then destroyed by permanently deleting all electronic data and cross-cut shredding of all paper materials associated with the study.
- The results of this study may be published.
By accepting the consent terms, you agree that you understand the nature of the study, the possible risks and benefits to you as a participant, and how your identity will be kept anonymous. Accepting the terms means that you are 18 years old or older and that you give your permission to volunteer as a participant in the study that is described here.
(☐) I accept the above terms. (☐) I do not accept the above terms. (CHECK ONE)
Appendix B
Questionnaire
Research Study
Thank you for your help with my study. The purpose of the study is to obtain information about your experiences to understand more clearly the process of adopting advanced medical-surgical technology through in-services or on-the-job-training. The questions should take about 20-30 minutes to complete.
Please describe your role/position in your current organization and department:
- Surgeon
- Anesthesiologist
- CRNA
- Surgical Technologist
- Other (please specify)______________________________________
From your experience, please explain the education and training you have received or continue to receive as a surgeon, anesthesiologist, CRNA, surgical technologist or “other” with the new medical-surgical technologies being employed.
- In-services
- On-the-job-training
- Online learning
- All of the above
Closing Remarks
Thank you again for taking time to complete this questionnaire.
Appendix C
Protocol for Data Collection
Hello, my name is Student, and I would like to thank you once again for agreeing to help and participate in this study. I am conducting a research study on the current training approaches, methods, and strategies used to determine the most preferred, most accessible, and most effective training approach to improve operating room staff competency with new medical-surgical technologies. Overall, the purpose of the qualitative descriptive design is to explore the training experiences of surgical staff for developing competency with new medical-surgical technologies.
The focus of the interview questions is on addressing the research questions as well as the study’s purpose. All names or identifiers will be removed during the analysis and presentation of data; you also have the right to withdraw your participation at any time or stage of the research process. We will first start with the background/ demographic information on your surgical role in the operating room. The Informed Consent must be agreed to before obtaining access to the questions.
Profession/Specialization:__________________________________________
Appendix D
Data Collection Protocol
Hello, my name is Student, and I would like to thank you once again for agreeing to help and participate in this study. I am conducting a research study on the current training approaches, methods, and strategies used in in-services and training to determine the most preferred, most accessible, and most effective training approach to improve operating room staff competency with new medical-surgical technologies. Overall, the purpose of the qualitative descriptive design is to explore the training experiences of surgical staff at the study site for developing competency with new medical-surgical technologies.
The focus of the questionnaire is on addressing the research questions as well as the study’s purpose. All names or identifiers will be removed by SurveyMonkey during the analysis and presentation of data; you also have the right to withdraw your participation at any time or stage of the research process. After you have accessed the questionnaire, you begin by indicating which surgical role in which you are employed followed by the interview questions.
Appendix E
Recruitment Flyer
Education and the Use of Medical Technology: A Qualitative Descriptive Study.
I am conducting a research study on Education in Medical Surgical Technology. I need YOUR help. Your participation will involve completing a web-based questionnaire available with any computer.
As EEEeeEasEeeeYou will log on to the SurveyMonkey to review and accept the terms of the informed consent form to be able to continue. As a participant, you may decide to withdraw prior to, during, or after completing the questionnaire. The time commitment for completing the Questionnaire is between 20 to 30 minutes.
The purpose of this research study is to obtain information about the experiences of surgical personnel who learn new, advanced, medical-surgical technology through in-services to acquire the acquired level of skill competency. Participants in the proposed study must meet the following criteria:
To qualify, you (a) will have experience working in surgery center, (b) will have attended in-services and on-the-job trainings on new technologies within the last two to three years.
The researcher will attempt to ensure that you have had experience with in-person/team-based training as well as technologically mediated training. In that way you can speak meaningfully about the advantages and disadvantages of either in-services or on-the-job trainings.
Anyone who is under 18 years of age, or does not fit these criteria, does not qualify. If you, by any chance, know of anyone who may be qualified, please pass this on to them. There is no known risk to participating in this study. Every effort will be made to protect the privacy and confidentiality of all elements of the study.
may be qualified, please pass this on to them. Thank you.
Although there may be no direct benefit to you, a possible benefit from this study is that the study may shed light on the means of enhancing knowledge and skill acquisition regarding the use of the modern technology. Participants may gain insight to the most effective training approach in operating room which may improve performance of surgical staff resulting in benefits to surgical patients as success rates in surgical procedures increase because of an effective training approach. I need at least 10 volunteers for my study whose names will remain anonymous. Here’s the link to the questionnaire on SurveyMonkey website.
THANK YOU!